High-tech treatment of open leg wounds no better than using regular dressings
- Study published in The Journal of the American Medical Association (JAMA) compared negative pressure wound therapy devices and traditional dressings
- Conducted by Warwick Clinical Trials Unit, the University of Warwick, University Hospitals Coventry and Warwickshire NHS Trust and Nuffield Department of Orthopaedics, Rheumatology and Musculoskeletal Science, the University of Oxford
- Results have implications for patients recovery and healthcare costs
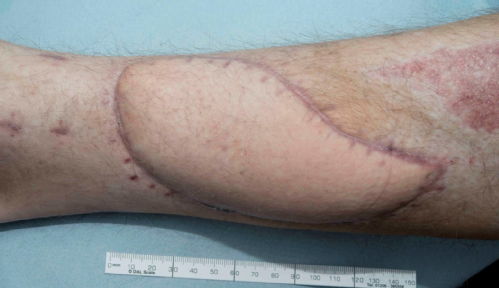
A new study of open leg fractures suggests there is no difference to patient recovery whether high-tech negative pressure wound therapy devices are used, compared to standard dressings.
The randomised clinical trial was conducted by the University of Warwick Clinical Trials Unit and the University of Oxford across 24 hospitals representing the UK Major Trauma Network. Their results Effect of Negative Pressure Wound Therapy vs Standard Wound Management on 12-month Disability Among Adults with Severe Open Fracture of the Lower Limb: The WOLLF Randomized Clinical Trial is published in The Journal of the American Medical Association (JAMA) on 12 June 2018.
This study was conducted on people with an ‘open’ fracture of the leg, where the bone has broken through the skin. The broken bone is exposed to contamination and there is a higher risk of healing-related complications. In severe open leg fractures, infection rates can be up to 27%. As well as affecting the recovery of the patient, infections can also increase healthcare costs due to longer hospital stays or extra treatments.
Negative-pressure wound therapy (NPWT) is a new type of dressing used after surgery. The device creates a vacuum using a suction pump which removes blood and fluid that may collect in a wound. The vacuum may also encourage the formation of granulation (healing) tissue. However, NPWT dressings and the vacuum machines are considerably more expensive than traditional wound dressings.
The researchers compared the level of disability, rate of infection and quality of life in 460 patients (the mean age was 45.3 years and 73% were men) with severe open fractures of the lower leg. It was not possible to do a ‘blind study’ of the participants and surgeons because the type of dressing was clearly visible. However the surgical and healthcare team were not involved in any outcome assessments. The primary method of measurement was a questionnaire given to the patients to rate their level of disability one year after they sustained their injury.
The research team found no evidence that the negative pressure wound devices reduced the patients’ disability at 12 months. The questionnaire results were 45.5 (negative pressure) vs 42.4 (standard dressings) points out a possible 100 where zero represents normal function and 100 complete disability. Wound photographs were also taken at six weeks. These were reviewed by independent clinicians who were not told which dressing was used. The research team found there was no evidence of a difference in the rate of deep infections, wound healing or patient quality of life.
Lead author, Matt Costa, Professor of Orthopaedic Trauma Surgery, Nuffield Department of Orthopaedics, Rheumatology and Musculoskeletal Sciences (NDORMS) said: “Our study did not find any benefit of using negative pressure devices in the treatment of these very serious injuries. Our research has implications for both patients and healthcare systems with regard to the management of severe open fractures. Just as importantly, the study also shows that UK patients and clinicians can work together to deliver high-quality evidence, even in the most difficult context of major trauma.”
Co-author, Professorial Fellow at Warwick Medical School, Professor Julie Bruce, said: “Before this study there was only one small randomised clinical trial comparing standard wound dressings with the devices which suggested negative-pressure wound therapy improved patient outcomes. However it was conducted at one trauma centre and only included 59 patients. Despite the lack of strong evidence, clinical guidelines around the world recommended the use of these devices for open fracture wounds. These guidelines will need updating.”
12 June 2018
Notes to Editors
Effect of Negative Pressure Wound Therapy vs Standard Wound Management on 12-month Disability Among Adults with Severe Open Fracture of the Lower Limb: The WOLLF Randomized Clinical Trial
Matthew L Costa PhD, Oxford Trauma, Nuffield Department of Orthopaedics, Rheumatology & Musculoskeletal Sciences, University of Oxford, Oxford, OX3 9DU, UK; Warwick Clinical Trials Unit, Warwick Medical School, The University of Warwick, Gibbet 1Hill Campus, Coventry CV4 7AL; University Hospitals Coventry and Warwickshire NHS Trust, Clifford Bridge Road, Coventry, CV2 2DX, UK
Juul Achten PhD Oxford Trauma, Nuffield Department of Orthopaedics, Rheumatology & Musculoskeletal Sciences, University of Oxford, Oxford, OX3 9DU, UK
Julie Bruce PhD, Warwick Clinical Trials Unit, Warwick Medical School, The University of Warwick, Gibbet Hill Campus, Coventry CV4 7AL
Elizabeth Tutton PhD, Warwick Clinical Trials Unit, Warwick Medical School, The University of Warwick, Gibbet Hill Campus, Coventry CV4 7AL; Oxford Trauma, Nuffield Department of Orthopaedics, Rheumatology & Musculoskeletal Sciences, University of Oxford, Oxford, OX3 9DU, UK
Stavros Petrou PhD Warwick Clinical Trials Unit, Warwick Medical School, The University of Warwick, Gibbet Hill Campus, Coventry CV4 7AL
Sarah E Lamb PhD Warwick Clinical Trials Unit, Warwick Medical School, The University of Warwick, Gibbet Hill Campus, Coventry CV4 7AL; Oxford Trauma, Nuffield Department of Orthopaedics, Rheumatology & Musculoskeletal Sciences, University of Oxford, Oxford, OX3 9DU, UK
Nick R Parsons PhD4 for the UK WOLLF collaboration Statistics and Epidemiology Unit, Warwick Medical School, The University of Warwick, Gibbet Hill Campus, Coventry, CV4 7AL, UK
Funding
This project was funded by the UK National Institute for Health Research Health Technology Assessment (HTA) Programme (project number 10/57/20) and was supported by the National Institute for Health Research (NIHR) Oxford Biomedical Research Centre and the NIHR Collaboration for Leadership in Applied Health Research and Care in Oxford.
Contact:
Tom Frew, Senior Press and Media Relations Manager – University of Warwick:
E: a dot t dot frew at warwick dot ac dot uk
M: +44(0)7785433155
