LGD 2004 (1) - Graciela Nowenstein
Organ Procurement Rates: Does Presumed Consent Legislation Really Make a Difference?
Graciela Nowenstein
PhD Candidate,
Department of Sociology,
European University Institute, Italy
Graciela.Nowenstein@IUE.it
Since transplantation became a mastered therapeutic tool in the 1970s, the problem of the shortage of organs has emerged as an important issue in public health debates. The supply of organs for transplantation has been organised around two systems of consent: presumed (opting-out) and express (opting-in) consent systems. Discussions have been going on now for more than 30 years about which of the two legal systems is likely to bring more organs for transplantation. No definitive answer has emerged from them. Actually, no definitive answer could emerge since debates have been going on in the absence of consistent data allowing thoughtful conclusions. It is very often written that opting-out systems of donation are more efficient than opting-in ones. In fact, if the hypothesis correlating donation systems with procurement rates deserves consideration, the data informing it appears to be unsatisfying. First, because it is based on inconsistent and not comparable data; second, because the legislative variable has been overestimated by many authors. Recent research is relegating the legislative variable to a secondary position and is focusing on the importance of organisational and structural variables. The authors who have followed this direction have not, however, proved the theoretical and practical irrelevance of legal systems of consent. The question about which is the set of variables accounting for procurement levels remains open, and in need of coherent comparative research.
Keywords: Express Consent, Law, Opting-In, opting-Out, Organ Donation, Organ Transplantation, Presumed Consent, Systems of Consent
Author’s Note
This article was written during my stay at the Social Sciences of Medicine department of McGill University. I would like to thank Margaret Lock, John Griffiths and Frédéric Mégret for their insightful comments.
This is a refereed article published on 4 June 2004.
Citation: Nowenstein, G, 'Organ Procurement rates: Does Presumed Consent Legislation Really Make a Difference ?', Law, Social Justice & Global Development Journal (LGD) 2004 (1), <http://elj.warwick.ac.uk/global/04-1/nowenstein.html>. New citation as at 15/07/04: <http://www2.warwick.ac.uk/fac/soc/law/elj/lgd/2004_1/nowenstein/>.
One of the miracles attributed to Cosma and Damian, the twin patron saints of physicians and surgeons, is that of having replaced the sick leg of a merchant with that of a dead servant in the 3rd century (Voragine, J, 1969). After centuries of experiments and research, modern medicine became capable, by the end of the 20th century, of mastering transplantation. Miracles were set to become technical routine. [1] Seen almost as magical feats in the era of the pioneers, grafting organs is nowadays pretty much a normalised activity, with its routine and even its scandals. Transplantation surgeons have been associated to petty affairs of corruption, organ traffic and abuses of authority. The activity nonetheless, remains surrounded by a veil of magic that has a lot to do with the very first and indispensable step of the transplantation process: that of the so-called ‘gift of life’ (Parsons, T, Fox, R and Lidz, V, 1972).
Even this last sphere, however, albeit partially, has gone through a process of disenchantment. Although the idea of the ‘gift of life’ has not disappeared, this area is nowadays more often evoked both in the media and in research literature under the disenchanted semantic fields of property, and of the (im)balance between the demand and supply of organs. In fact, it has become a common place in the literature on transplantation that the strongest impediment to this activity nowadays is neither medical nor technical, but institutional or societal. In countless articles, books, and conference panels, the idea of the ‘gift of life’ has been replaced by a reflection increasingly labelled in terms such as: ‘Expanding the donor pool’ (panel at the European Transplant Coordinators Organisation, Annual Meeting, 2002), ‘Improving organ retrieval rates’ (Kluge, E H, 2000), ‘Incentives for organ donation’ (Kittur, D S et al, 1991), ‘Do we own our bodies?’ (Calabresi, G, 1991), etc.
The mismatch between demand and supply has encouraged the media, medical professionals, political actors, legal scholars, philosophers, and social scientists, to try to figure out how to solve – or at least reduce – what is seen in many countries as a problem of public health. Such reflection seems all the more needed given that some countries are significantly more successful than others. [2] Indeed, although in all countries practising transplantation patients die while waiting for an organ, the records are not equally tragic everywhere. To give just one comparative illustration, 16.7 percent of patients from the heart waiting list die every year in the Netherlands, while ‘only’8 percent do so in Spain. [3] What might be the factor(s) explaining this difference? Can it/they be applied to different national realities?
The factor one finds most commonly at the heart of the existing debate concerns the legal regime applicable to consent to organ donation. [4] It seems at a first glance that the situation is more favourable in countries where the legislator has chosen an opting-out system of consent to organ donation rather than an opting-in one. Under opting-out regimes, the law considers that those persons who have not expressed their opposition to donation while they were alive are willing to donate their organs. These systems are based on a presumption that individuals are willing to donate their organs, and are also called presumed consent systems. Under opting-in, or express consent, systems, on the contrary, only those patients who, before death, have expressed a will to donate, are considered donors (Somerville, M A, 1985).
If the hypothesis correlating better donation rates and the choice of the legal system organising organ procurement does deserve consideration, this article will show that the relevance of this correlation has often been overestimated. In fact, this is because although the two systems are formally opposite, the frontier between the two is hazy in practice, where the formal opposition is diluted(2). Which, then, might be the other factors that matter in determining procurement rates? Unfortunately, the existing data does not make it possible to answer to this question because it is incomplete and too incoherent to allow transnational comparisons and generalisations. There is a clear need for in-depth analysis of national cases that should be filled in the following years. The description and analysis of the French case, based on qualitative research (including interviews, analysis of legislative and media sources) (3) will show how this sort of analysis can enrich the debate on the relation between formal normative systems of consent and practical outcomes (4).
2. The Claimed Superiority of Presumed Consent Systems
2.1.1 Cadaveric Donors and Heart-Beating Dead
Before one goes any further, it should be stressed that this article will only treat the issue of consent in relation to cadaveric donors, both because living and cadaveric donations raise different questions, and because in most countries a large majority of organs for transplantation come from cadaveric donors. [5]
Moreover, it is worth mentioning that not all corpses are eligible as sources for transplantation. Organs [6] are mainly taken from a specific kind of cadaver, that is, from patients who have been diagnosed as brain dead. A brain dead patient is someone who, generally after a road accident or a stroke, has had an internal haemorrhage that has caused irreversible damage in the brain. This occurs because the brain has swollen until blood can circulate no longer, and therefore until it ceases to be oxygenated. As a result, the brain stops functioning, something that is fatal to the rest of the body. The rest of the body’s functions, however, can be kept working for some time with the help of drugs and artificial ventilation. At this stage, the person is said to be dead, and this is why the brain dead are also referred to as ‘heart beating’ dead (Carvais, R and Sasportes, M; 2000). The reason why organs are taken from these cadavers rather than from ‘normal’ ones is that the time of non-oxygenation of organs is reduced to the minimum, i.e.: to that of extraction and transportation. This means that organs will suffer less damage, and better transplantation results will ensue (Carvais, R and Sasportes, M; 2000).2.1.2 The International Consensus on Consent
There exists an international consensus about what basic ethical requirements the cadaveric systems of organ donation should fulfil. It is admitted that systems of collection and allocation of cadaveric organs should not be organised under the rules of the market, and that it is necessary to obtain some consent before proceeding to retrieval. Both models of consent, presumed and expressed, are based on the principle that the wishes of the deceased should be at the basis of the decision to opt-in or out, and that it should be respected (Schneider, W; 1999). Both are considered to be acceptable. The World Health Organisation established in 1991 that:
Organs may be removed from the bodies of deceased persons for the purpose of transplantation if:
(a) any consents required by law are obtained; and
(b) there is no reason to believe that the deceased person objected to such removal, in the absence of any formal consent given during the person’s lifetime (WHO, 1991) [7] .
One or the other system of consent has been generally adopted by those countries that have legally regulated cadaveric donation, even though the tendency seems to be towards an increase in the number of countries where opting-out systems are adopted. Countries such as Great Britain, the USA, Ireland, Germany, the Netherlands or Sweden have opting-in systems; whereas countries such as France, Spain, Norway, Portugal, Austria, or Belgium have based their legislation on the second model.
Why have these countries opted for one or the other system? Is this only a choice of moral preferences, or is one of the two systems more efficient than the other (ie does it bring more organs for transplantation?)?
2.2 The Best Donation Rates Come from Presumed Consent Systems
There seems to emerge from most of the existing literature a consensus that opting-out systems are more efficient than opting-in ones. Indeed, if anything the latter are defended on ethical grounds rather than efficiency ones (see for instance Kluge, E H, 2000) and also Calabresi, G, 1991). The following chart shows the 2002 procurement rates of countries with express consent -in blue- and presumed consent -in pink [8] :
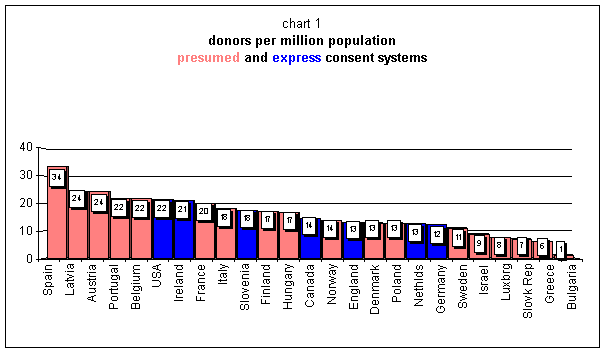
What does this chart show? To be sure, the five most successful cases are countries with presumed consent legislation. [9] In fact, Spain, Belgium and Austria are almost systematically cited as examples of the superior efficiency of systems of presumed consent in the literature. Above all, it is the Spanish case that is showcased as evidence that presumed consent legislation is better at fulfilling the aim of augmenting the procurement rate, and it has now become a common place to talk of ‘the Spanish model’.
2.3 Is the Generalisation of Presumed Consent Legislation the Solution to Shortage?
2.3.1 Lobbying in Favour of Legislative Change
It has been just noted that a consistent strand of the literature considers presumed consent legislation to be more efficient. Provided it has been agreed that presumed consent is morally an acceptable option, and if lawmakers are willing to contribute to increasing the number of organs available for transplantation, this means that opting-out systems should be generally adopted. The British Medical Association, for instance, has in the last years called for a modification of the express consent British legislation towards a presumed consent system (British Medical Association, 2003). Even in countries with less developed health systems there is considerable support for this option: in Mexico, a draft law was submitted in 2000 with the aim of adopting a system of presumed consent (Brena Sesma, I, 2002); and Argentinian legislators should vote in favour of such a system in 2004 [10] .
2.3.2 Towards a More Pragmatic Support of Presumed Consent Legislation
If articles in the 1980s and beginning of the 1990s were usually naively optimistic about the possibilities of increasing organ donation by adopting presumed consent legislation, emphasising the existence of rather linear and neat causal relations between law and results, the tone changed by the mid 1990s. Nowadays, even those who defend the presumed consent option do so in a more nuanced way. [11] The following quotation from the British Medical Association is a good illustration of this trend:
Despite the acknowledged difficulties of obtaining meaningful data about the success of presumed consent in other countries, the British Medical Association (BMA) believes that, as one part of a broader strategy, a shift to presumed consent is likely to have a positive effect on donation rates. (British Medical Association, 2003) [12] .
Indeed, it has become common to qualify support for presumed consent systems with the idea that other variables are also to be taken into consideration in the analysis of the efficiency of donation systems. A good example of these more subtle expressions of support to presumed consent is an article published in The Lancet in 1998 by a multidisciplinary team of prestigious physicians and researchers in humanities and law arguing in favour of presumed consent (Kennedy, I et al, 1998). The authors acknowledge that there is a set of non-juridical variables that can be said to influence organ donation rates – such as organisational aspects of organ procurement, or education and information policies among others. These authors, however, still adhere to the belief that the legislators’ choice between the two systems of consent does matter because, they note:
In three western countries there is evidence that changing to a contracting out system resulted in an increase in organs – Spain, Austria, and Belgium – …
There does indeed seem to be, if one goes back to Chart One, a correlation between legislation and efficiency of procurement systems, and it seems a priori difficult to argue against such an apparently evidence-based statement, for it is true that the five best procurement rates are from presumed consent systems. But it also seems important to be a bit sceptical and question the principal postulate behind most statements in favour of presumed consent, namely that there is a linear causal link between presumed consent regimes and better procurement rates.
Why should one challenge this postulate? First of all for the methodological reason that an independent variable is not pertinent simply because there seems to be a correlation between it and the fact one wants to understand. The social process at stake here is a very complex one, and one should be prudent when generalising about the relevance of one variable that coexists with a myriad of others. One should be even more prudent when entering the risky waters of transnational comparison. Second, because there has been in the last few decades a considerable amount of substantial research and literature in social sciences and in legal studies expressing profound scepticism about the idea that there is such a thing as a linear relation between the law and social behaviour. [13] Questioning the postulate that the choice of the legislator seriously determines the shape things take in practice seems the least one can do in light of that literature.
2.4.1 Shortcuts in Data Analysis
Let us begin by pointing out that things are much less clear than the data in chart 1 seems to suggest a priori. If one removes the opting-in countries, it becomes substantially less clear that the law is having an effect on behaviour. Indeed, if the highest donation rates are among countries with presumed consent systems, so are the lowest ones [14] :
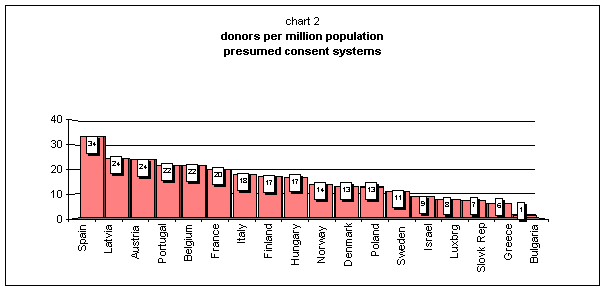
To add to the confusion, if one extracts the Spanish case from chart 1, the difference between the two systems becomes even less clear-cut:
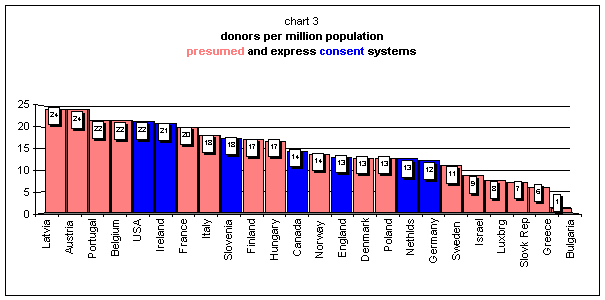
To be sure, there are still differences between the first presumed consent countries and the first express consent ones: Latvia and Austria have 24 donors per million population, and the USA and Ireland, as the first two among express consent, have respectively 22 and 21. Yet, such differences do not seem to be significant enough to allow a credible inference between law and social behaviour. Not to mention that the differences between Portugal and Belgium on the one hand, and the USA and Ireland on the other are simply too marginal to be conclusive. [15]
2.4.2 Weak Evidence Sustaining the Superiority of Presumed Consent Systems
The Belgian case has attracted a lot of attention as being one of the most successful cases of rapid increase of organ procurement thanks to the passing of presumed consent legislation. The literature on the Belgian case has evolved in its way of interpreting the link between presumed consent legislation and good donation rates. From a linear and somewhat naïve view in the beginning of the 1990’s (Roels, L et al, 1990; Roels, L et al, 1991), an evolution towards a much more complex approach is evident (Michelsen, P, 1996). Michelsen (1996) points out that the Belgian results cannot be understood without relating them to the implementation of a decentralisation policy that has in his view played a very important role in procurement results.
The decentralisation variable actually appears to be an important factor in the eyes of authors who are at the core of procurement processes in successful presumed consent countries (Michelsen, P, 1996; Gnant and Muhlbacher, 1990; Matesanz, R, 2001). Michelsen (1996) also evokes decentralisation as one of the important explanatory variables of the Austrian success, and observes that the increase of organ donation rates significantly postdates the passing of the presumed consent law there. Indeed, the law was passed in 1981 but:
The number of donors did not change until 1984, when a decentralized model of donor procurement was developed in Vienna and Linz and led to a 100% increase in these two centres (Michelsen, P, 1996).
It has been confirmed by Austrian physicians who have written in The Lancet that:
The ‘presumed consent’ law and the high rate of fatal accidents in Austria are not the only explanations for this success because both conditions have been present since 1982 while the current trend did not set until 1986. Furthermore … our rates are much higher from other countries with an opting-out law (Gnant, M F X and Muhlbacher, F, 1990).
These arguments weakening the hypothesis of the centrality of presumed consent do not lead the authors to reject the idea that the legislation variable should be considered. Michelsen (1996), for example, after pointing at the decentralisation process as an important variable, still maintains that the presumption of consent is relevant to the Belgian results. Legislation on presumed consent does seem to have helped to cultivate a strong feeling of autonomy among the professionals in charge of the procurement and donation processes. This, in turn, has had an influence on the procurement rate.
In fact, what sticks out in Michelsen’s (1996) article as being important about presumed consent legislation is that it has contributed to a sort of normative and policy context which creates a state of mind that is conducive to obtaining organs. The problem, of course, is that at this level of analysis and without consistent qualitative research to substantiate these claims, it is difficult to establish anything except a strong intuition that presumed consent legislation might be having a relevant effect.
This having been said, is there in these examples enough counterevidence to invalidate the hypothesis of a correlation between the legal system of consent and the procurement outcomes of a country? Although the picture emerging from Belgium and Austria is blurred, it might be too hasty to argue that presumed consent legislation is useless as a tool of socio-legal engineering. Perhaps if it were proved that the ‘Spanish model’ owes its success to presumed consent, then the hypothesis would gain renewed vigour.
2.4.3 The ‘Spanish Model’
Here is what Matesanz, founder and first director of the Spanish Organización Nacional de Transplantes, wrote in 2001 about presumed consent in Spain:
There are many countries trying to increase organ donation ... and are many discussions about ‘presumed consent’ or ‘opting out’ laws.
... when the ONT [Organización Nacional de Trasplantes] was created, there were many people in Spain who believed that the main solution to solving the problem of organ shortage was to ... apply a strict presumed consent law. However, we found little evidence to suggest that the style of legislation influences the organ donor because regardless of how the donor might become available, relatives are always consulted, as in most European countries, and their wishes are always respected (Matesanz, R, 2001).
Actually, if one looks closer at Spain’s success, one notes that the good results do not start with the passing of the law, which goes back to 1979. The beginning of a significant increase in procurement rates is noticeable from 1989 (Matesanz Acedos, R and Fernandez Lucas, M, 1996). From then on the increase has been impressive, moving from 14.3 donors per million population in 1989 to 33.7 in 2002. [16] 1989 is not a neutral date. In fact, it is the year when the ONT was created, and when this strong organisational and institutional machine started regulating and supporting all activities linked to transplantation in Spain. [17]
Matesanz (2001), after denying the legislative frame any significance, explains what he sees as central to the success of the so-called ‘Spanish model’; which in his view has its roots in a whole set of variables. Among them are said to be important organisational and structural aspects, including a multi-level system of hospital coordinators in charge of coordinating and organising the donation and procurement processes at national, regional and local levels; an efficient system of detection of brain death cases [18] ; a developed training system where hospital coordinators are taught how to interact with the relatives of potential donors as efficiently as possible; a very professionalised approach to public relations, especially as regards the media (hospital coordinators are for instance trained in public relations, in what to say in public and what not, etc). Finally, he adds variables at the more general level of the national health care system are to be considered such, as the number of ICU beds, the amount of money a procurement process costs to a hospital, etc. These are the aspects that in his view other countries might be wise to reflect on if they want to increase their donation rate significantly.
If the man who is known as having been at the heart of the Spanish success writes that the latter owes nothing to the presumption of consent, should one be inclined generalise this statement and conclude that the choice of legal system is a non-pertinent variable? That the choice of the legislator simply does not matter? That a substantial part of the relevant literature in the field is misguided, even wrong?
It might be tempting to do so. But in so doing one would run into the same mistake as those who have overestimated the general efficiency of presumed consent systems. To be sure, the Spanish case does once and for all invalidate the vision of a neat and direct correlation between legislation and practice, between the law supposed to regulate organ procurement and procurement rates themselves. In that sense, what can be concluded at this stage at the very least is that it is not possible to state that presumed consent legislation guarantees good donation rates.
Nevertheless, it remains quite another matter to prove that, in all presumed consent countries, ceteris paribus, the law is irrelevant. The data presented until now would need to be completed by in-depth analysis of national cases where the structural, institutional but also contextual specificities would be brought together to obtain a more detailed picture of each country. In the absence of this sort of study, no serious comparative analysis can be embarked upon. This sort of data is, unfortunately, lacking. The following sections present an illustration of what these analyses could reveal about the hazy relation between law and action in the sphere of organ donation. They will be centred on the description and analysis of the French case, at the core of the author’s current doctoral research [19] .
3. The Tension Between Law and Practice in France
3.1 One of the Oldest Presumed Consent Legislations
To give the general picture succinctly, France has one of the oldest presumed consent legislations. The first law was passed in 1976 [20] ; the presumption of consent was confirmed in 1994 by a vote in Parliament, and should be so again in 2004 [21] . The interesting thing, however, is that this periodic and almost ritual confirmation of the law occurs despite the fact that the legislator has been regularly informed that the law is not applied precisely by those who are supposed to (see for instance Claeys, A and Huriet, C, 1999) [22] . Public authorities, it seems, do attribute a certain importance, at least symbolically, to the legislation on presumed consent in public discourses and legislative debates. Last but not least, the actors of the field (hospital coordinators –nurses- and intensivists) who are supposed to be the arm of the law display apparently paradoxical inclinations. On the one hand, they make it clear in the interviews conducted by the author that ‘presumed consent’ is not applied, even though they are aware that the legislator has put at their disposal what is potentially a powerful tool in obtaining organs. On the other hand, they claim to be keen on the law and opposed to switching to a regime of express consent law, even though such a law would better reflect their actual practice.
The following sections focus on this tension. Indeed, it seems important to move away from the legal normative structure as such, and to concentrate instead on how it interacts with other sources of normativity that seem to be a better key to the behaviour of those in the field.
3.2 1976-early 1990s: From Disorder to Standardisation
3.2.1 A Messy Start
The ‘older’ intensivists and hospital coordinators interviewed, namely those who have been involved in procurement activities since its early years – mid 1970s-early 1980s – agree that things have considerably changed since the first enactment of the presumption of consent in 1976. This is so as regards not only the degree of application of the law, but also the homogenisation of behaviours. According to them, there were no generalised rules of behaviour until the beginning of the 1990s. Until that date some units would apply the presumption of consent and some not; even within the same unit, all professionals would not behave alike; in some hospitals it was transplantation surgeons who would come to the ICU where the potential donor had been declared dead and solicit the relatives for donation; in some units the relatives were put under pressure to accept donation, and in others not; in some units the relatives were simply not informed about the harvesting. [23]
The different experiences of two ‘old’ hospital coordinators illustrate the diversity of approaches during the first fifteen years of presumed consent legislation in France. Both describe how things were in two of the bigger procurement and transplantation centres of Paris and its surroundings.
Hospital Coordinator A remembers that in her unit the relatives of potential donors were not asked about the retrieval or, if they were, the question was asked so unclearly that they could not truly understand what they were being asked. She reports that, after the announcement and explanation of brain death, they would be asked something like: ‘Do you happen to know what the wishes of the deceased were?’ [24] Not knowing what the staff was talking about, and being in a state of affective shock and at the beginning of a sudden grieving process, the usual answer was a vague ‘No’. As she acknowledges, this way of doing was not only ‘hypocritical’, it was also ‘dishonest’. It also made it somewhat dishonest to talk about ‘acceptance’ and ‘refusal’ rates for this period, at least in the hospital she was working at. There are three reasons to that: (a) the general population was not aware of the existence of an opting-out system. Therefore, they could not even conceive of the possibility of opting-out before dying; (b) even if some citizens happened to be informed about the legislation, there was no official way of registering one’s wish to opt-out; (c) the relatives were not asked specifically about what the deceased might have wanted in the circumstances. From today’s perspective she sees this as morally wrong [‘dishonest’ and ‘hypocritical’], but the staff involved in the activity knew the law of presumed consent was protecting them, and somehow allowing this sort of behaviour.
The experience of Hospital Coordinator B is different. In charge of procurement and donation, also in a university hospital, she says she always had a meeting with the relatives of the brain dead and always respected their position. She says this caused her some problems with transplantation surgeons who scolded her for not respecting the law. She persisted in this practice with the support of her unit head. It is noteworthy that her procurement rates have always been pretty high and are nowadays above the national mean.
3.2.2 The Beginning of a Normalisation Process
The ‘old’ interviewees concur that things changed by the end of the 1980s and the beginning of the 1990s. By that time the country had gone, and was going, through a series of major scandals in the area of health policy, some of which involved organ procurement. First of all there was the so-called ‘contaminated blood scandal’, starting in 1985, where political and health authorities, and physicians, were accused of not having prevented the transfusion to haemophilic patients of blood contaminated with HIV virus. Smaller scandals directly linked to organ procurement and transplantation also damaged, in the view of the interviewees, the image of medical professionals and generally of those working in health institutions. One, revealed by the press in 1992, concerned the ‘abusive’ harvesting of a young man of 19 year-old; another concerned the unequal allocation of kidneys in a big nephrology unit in 1993.
The case of the teenager was given a great deal of attention in the media. The following was reported: in the city of Amiens, a 19 year-old teenager was killed in a road accident; once declared brain dead the parents were asked for authorisation for organ donation, even though, being over 18, the teenager fell under the presumption of consent; the parents accepted the retrieval of some of their son’s organs; later they accidentally learnt that much more than what they had authorised had been extracted from the body of their son. What shocked them most was that the hospital staff had taken the ‘eyes’ of their son and had apparently sewed back his thorax with wire. Of course the hospital staff involved was protected by the existing laws and successfully defended the litigation launched against them by the parents. Yet, the case was in the media for a long period and the medical profession was depicted in very negative terms. [25]
During this same period, urban legends flourished about organ stealing, selling and traffic at the national and international levels. Whether generally true or not (Campion-Vincent, V,2000; Scheper-Hughes, N, 2000), these rumours seem to have considerably damaged the image of the professionals involved in procurement and transplantation activities.
It was in this general context, the interviewees note, that more and more centres started normalising the inclusion of families in the procurement decision-making. It seems that from the mid-1990s onwards, families were being consulted in most of the harvesting centres. This standardisation of practice was confirmed by a modification of the law in 1994.
3.3 1994: The New Law, Between Ambiguity and Clarification
3.3.1 The Exclusion of Transplantation Surgeons from the Donation Process
It soon appeared in the travaux préparatoires of the 1994 law that transplantation surgeons had to be insulated from the families of potential donors. Because they were seen as too keen on obtaining organs, it was considered that entrusting them with the donation decision and involving them directly in discussions with the families presented too big a risk of abusive and incorrect behaviour. Waissmann’s (1996) article based on interviews with relatives of brain dead patients confronted with requests for donation before the change in the law illustrates the rudeness which some transplantation surgeons demonstrated in these discussions.
3.3.2 The Introduction of the Family in the Process
The first French presumed consent law passed in 1976 belongs to the category of strong presumed consent systems (Machado, 1998) where the law gives no role to the relatives of the potential donor, not even as a vector of information about the deceased’s will. In 1994, however, the legislators added a section that made the system switch to one of soft presumed consent. The section said that in the absence of any information about the wishes of the deceased, the hospital staff has to do its best to search for this information by asking the next-of-kin of the potential donor. [26]
3.3.3 An Official Device to Opt-Out
A third addition in the 1994 law was that it anticipated the creation of a registry of refusals meant to clarify and reinforce the presumed consent device in two ways. On the one hand, the idea was to avoid mistakes and abuses that might lead to the retrieval of organs from potential donors who, while opposed to donation in their lifetime, had not had a formal opportunity to record their opposition. On the other hand, the registry was also supposed to facilitate the application of the presumption of consent, since non-registration could more clearly be interpreted by the hospital staff as evidence of the potential donor’s lack of opposition.
The interesting thing, however, is that this clarification was only partial. Indeed, coming on top of the inclusion of the next-of-kin, the law seemed to create two parallel sources of identification of the deceased’s consent: the registry, and the family. Substantial ambiguity resulted from this doubling-up (Thouvenin,1997). One could say that, strictly speaking, the section introducing the family does not give the relatives any particular power, since they are nothing more than a vector of information about the wishes of the deceased and are not supposed to be asked about what they themselves would wish. But, as intensivists and hospital coordinators point out, it is far from easy once one has started an exchange with the relatives about the wishes of the deceased, simply to exclude them from the decision-making process.
Might this ambiguity be a possible explanation for the non-application of presumed consent by French hospital coordinators and intensivists? It does not look like it judging by the interviewees’ accounts, and they do not identify it as a problem. In fact, they consider it is absolutely normal to take the decision of donating with the relatives of the potential donor.
If this formal ambiguity does not seem to be causing the non-use of the presumed consent device, let us now turn to the reasons they in fact give to explain this process.
4. Law as Text and Law in Practice
4.1 Reasons Not to Apply the Presumption of Consent
The reasons invoked not to apply the law are of three sorts: pragmatic, principled, and others that could be said to belong to the domain of professional ethos.
4.1.1 ‘We Can’t Do It’
The first point the interviewees make is that the State, or the collectivity in general, does not enjoy enough ‘power’ to impose this sort of burden upon citizens because this would be seen as abusive by the general population. In fact, in their view, families would be so deeply shocked if things were done strictly according to the law that, after a few months of strict application of the presumption of consent, public scandals and law suits would have the perverse effect of provoking a massive registration of unhappy citizens in the registry of refusals, not to mention the further loss of prestige of medical and political institutions.
Another reason for scepticism about the law’s applicability is what they refer to as ‘the end of paternalism’ in doctor/patient and doctor/family relationship, a phenomenon of recent decades whereby families and patients have demanded greater participation in health institutions.
4.1.2 ‘It Would be Wrong to Do It’
Apart from these pragmatic reasons, French intensivists and hospital coordinators also evoke more value-oriented justifications. Most of them say they go through a strong process of identification with the families of potential donors. If they were in the next-of-kin’s situation, they reckon that they would definitely resent it if the state were to impose the retrieval of organs on the basis of overarching community interests. Some of them go as far as to point out that they do not really know whether they would accept the harvesting of the organs of a potential donor belonging to their family, even if there was no evidence of any opposition to it.
Referring again to the public scandals mentioned above, they also note, despite the difficulties it might create in their everyday practice, that they share, or at least understand, the impulse that has lead to a modification of the relation between the general population and medical professions. Some of the old hospital co-ordinators who used to work in units where the families were either not informed, or not well informed about organ donation, consider it would nowadays be immoral to do such a thing.
4.1.3 Professional Ethos: Medical Professionals and the Law
One of the striking things to emerge from the interviews is that interviewees often do not seem to consider that situations where laws are not applied are per se problematic in the first place. Indeed, they seem to see the non-application of some laws as a banal occurrence, and a problem only to those who live removed from real life. It is true that, structurally, the medical profession has traditionally enjoyed a considerable amount of autonomy as to the regulation of its activities. The head of an intensive care unit illustrates this idea when he points out that, in their everyday activity, physicians often ‘sit on the law’. Actually, they are prone to look for guidelines for action from professional and/or personal values.
Two things buttress these professionals’ claim for autonomy. First, the idea that laws are not to be followed merely because they are legal rules; second, the fact that the legislator is often ill-placed to promulgate laws affecting professionals’ activity in the first place. In their accounts interviewees often disparaged legislators for lacking the necessary knowledge of the field or the activity which they seek to regulate, knowledge that can only come from an everyday contact with the situations professionals have to face.
Do the interviewees conclude, from this general description, that it would be wise to adapt the legal text to practice? Their answer seemed to be ‘why bother?’ They could not think of any legislative change that would increase the donation rate. And if not for this reason, why should energy be wasted in modifying the law?
In fact, at this point in the interviews they often stressed that the situation is not that bad, that the law is, after all, ‘a good law’. Why is this so?
4.2 Reasons to Keep the Text as It Is
4.2.1 The Law Gives Shape to the Dialogue
The interviewees are absolutely sure that the law cannot have the social fate the legislator dreamed for it. But they do admit it might be of some help in their activity. First of all, they note, because it gives them the possibility to channel the discussion with the relatives in a way they think is more advantageous than that which a law of express consent would allow. Two areas are here emphasized: the wishes of the deceased rather than that of the members of the next-of-kin on the one hand and the supposed generosity of the deceased on the other.
This may seem contradictory after having made it clear that the presumption of consent of the deceased is not applied in practice and that the family will usually have the last word. The point the interviewees make, however, is that although most of the time the family will have the last word, the law of presumed consent frames the discussion at its beginning towards what could be called the ‘fiction of the centrality of the wishes of the deceased’. The donation issue is addressed to the family in the first place more or less in the following terms: ‘Do you happen to know whether the deceased ever expressed opposition to giving her organs for transplantation?’ The usual answer is ‘no, we never discussed it’. At this point, note the interviewees, the natural tendency would be for the wishes of the next-of-kin to take over. Yet, the first question gives the professionals in charge the opportunity to go back to the fact that the deceased never expressed opposition to donating.
This facilitates a positive exploration of the personality of the latter, which will be launched by the hospital staff, often with something like: ‘You tell me/us she never mentioned an opposition to donating, was she generous? Did she for instance donate blood? Would she generally think it was important to help others?’ etc. It has been noted above that both opting-in and opting-out systems are based on a presumption about the wishes of the deceased. To be sure, these questions the French staff asks the next-of-kin are shaped by the presupposition of donation. However, the most one can conclude from this sort of accounts is that the presumption of consent might be a slight facilitator. But when one knows that the French donation rate is lower than those of express consent countries such as Ireland or the USA, it is difficult to establish a general conclusion about this. Or at least one might think that the legislative and policy effort should be concentrated on more important factors that seem to have proven more efficient in increasing procurement rates.
4.2.2 It is Symbolically a Good Law
Indeed, despite the marginal positive effect presumed consent legislation might have, it remains unclear why these professionals are so attached to a legal text they claim not to really use. Two things are to be added here to complete this general picture. The first is that, despite their identification with the families, the interviewees also share the ideal of society that inspired the legislator when passing the legislation on presumed consent. They are, after all, public service workers and seem to have a strong sense of public duty and public solidarity. As such, they consider it ‘normal’ that solidarity should be at the core of legal norms. This does not stop them from acting with self-restraint, consideration and pity when faced with a grieving family. Yet, it seems that the presumed consent law is important in echoing a normative and positive vision of society they generally share.
In fact, this seems to be one of the reasons why legislators have confirmed the law in 1994 and will certainly do so in 2004 despite its persistent non-application: this law tells a pleasant tale about French society, a tale of solidarity and maybe even progress.
This article does not aim to reach solid conclusions, even less offer solutions. It is more interested in sowing doubt about the neatness and the linearity of the correlation between law and action in the literature about organ donation and procurement, a correlation that is too often taken for granted. All one seems authorised to say on the issue on the basis of existing data is that law seems sometimes to matter a little and sometimes not at all. Another point that emerges is that when the law does matter, it does not necessarily do so for the top-to-bottom, instrumentalist reasons that are often ascribed to it. Rather, if and when the law matters, it seems to be for reasons that only appear once the law has been let out in the real world, when real actors appropriate its meaning and transform it into tools adapted to their institutional context and the situations they have to deal with every day.
Endnotes
[1] In the history of transplantation the early 1980s mark an important crossroad. By that time, the technical aspects were mastered but life expectancy was low due to the insufficiency of immunological knowledge in the medical sciences. In fact, the organisms of grafted patients were too often and too quickly rejecting the new and alien organ. A new anti-rejection substance, ciclosporine, was going to considerably improve the situation in the early 1980s by extending considerably life expectancy after transplantation.
[2] To be sure, countries that can be considered for comparison in this area are generally western developed ones. Some examples not coming from this area will be evoked, but this article is mainly inspired by countries having reached a certain level of biotechnical development and wealth.
[3] <http://www.msc.es/ont/esp/estadisticas/f_estadisticas.htm>
[4] Journals such as The Lancet, Transplantation, or Transplantation Proceedings concentrate a lot of the existing reflection on the issue. If a considerable amount of the authors writing on the issue are from the medical field, not all are, and social scientists, legal and bioethics scholars have also contributed interesting insights.
[5] For instance, in Europe, 91.5 percent of kidneys come from cadaveric donors, and 75 percent in the USA (Carvais and Sasportes, 2000, p 219)). There exist national variations, but it is generally estimated that in the United States of America the living donation rate is one of the highest – with the exception though of Norway, where more than half of the grafted kidneys came in 2003 from living donors <www.scandiatransplant.org>. More generally, it is estimated that 98 percent of the organs transplanted in the year 2000 in Spain came from cadaveric donors (López-Navidad and Caballero, 2001, p 795).
[6] The argument applies to procurement of both organs and tissues. However, for convenience we will refer throughout to ‘organs’ rather than ‘organs and tissues’.
[7] See also the Council of Europe (2002), Article 17: ‘The removal shall not be carried out if the deceased person had objected to it.’
<http://conventions.coe.int/Treaty/EN/Treaties/Html/186.htm>
[8] The rate generally used in these pieces give the number of donors per million population (pmp). The chart has been composed out of procurement rates of the year 2002 coming from Spanish Organizacion Nacional de Trasplantes <http://ww1.msc.es/ont/esp/estadisticas/f_estadisticas.htm>. Rates, originally with two decimals, have been rounded out.
[9] Not rounded off, the three countries showing 22 donors pmp have the following rates: Portugal, 21.7; Belgium, 21.65; USA, 21.5.
[10] ‘Consentimiento presunto - Modificaciones a la Ley Nº24.193. Proyecto de Ley, Buenos Aires 25 de febrero de 2003’ <http://www.incucai.gov.ar>.
[11] See the evolution in that sense between articles evaluating the Belgian case between 1990 and 1996: Roels, L et al, 1990 and 1991; Michelsen, 1996..
[12] In practice, relatives are solicited for consent in the United Kingdom, although the law does not oblige medical staff to engage in this consultation (Human Tissue Act 1961).
[13] The ‘founding fathers’ of sociology themselves, such as Durkheim (1968) and Weber (1971), questioned the existence of a linear connection between law and social action. As regards the legal field specifically it would tedious to refer here to the enormous quantity of literature produced by the so-called ‘law and society’ school. To quote only one, see Macauley’s founding article (Macauley,1963).
[14] To be sure, the very lowest rates (Bulgaria, Greece, Slovak Republic) come from countries with a low overall transplantation activity.
[15] Rounded off in the chart these rates are: Portugal, 21.7; Belgium, 21.65; USA, 21.5, Ireland 21.05.
[16] <http://www.msc.es/ont/esp/estadisticas/donacion/dona10.htm>
[17] The ONT was created by law in 1980, but it only started functioning in 1989. See <http://www.msc.es/ont/esp/informacion/f_informacion.htm>
[18] The problem of ‘unreported’ cases of brain death is a major one in many countries trying to increase the number of available organs for transplantation. All the unreported cases are unexploited cases of potential procurement.
[19] This research is still ongoing and is based on data gathered since the year 1999. It consists on in depth interviews done with hospital coordinators (nurses in France) and intensivists in charge of the procurement process in their hospitals and working in the Parisian area. A survey has been done at the national level with hospital coordinators about how they perceive their function and role. Besides, legal and parliamentary debates have been analysed, as well as the media following of organ donation and transplantation issues.
[20] ‘Loi ‘Caillavet’ du 22 decembre 1976’.
[22] French Parliament has an office in charge of the evaluation of the laws regulating science and technical activities, among which are included all the so-called biomedical regulations, the Office Parlementaire d’Evaluation des Choix Scientifiques et Technologiques.
[23] Interviews. See also for testimonies from relatives of potential donors in the 1980s see Waissmann, 1996.
[24] ‘Avez-vous connaissance de volontés exprimées par la personne de son vivant?’
[25] See for instance Le Monde, 17-18/05/1992, ‘La mort violée’; Le Parisien, 18/05/1992, ‘Vol d’organes: Une famille accuse’; L’evenement du jeudi, 20/05/1992, ‘Plus jamais ca!’; Le Canard Enchaine, 20/05/1992, ‘Dernieres nouvelles du cannibalisme’, etc.
[26] ‘Si le médecin n’a pas directement connaissance de la volonté du défunt, il doit s’efforcer de recueillir le témoignage de sa famille.’ Loi n° 94-654 du 29 juillet 1994 relative au don et à l’utilisation des éléments et produits du corps humain, à l’assistance médicale à la procréation et au diagnostique prénatal’.
References
Brena Sesma, I (2002), ‘Reflexiones Juridicas en Torno a Los Sujetos que Intervienen en un Trasplante de Organos’, Boletin Mexicano de Derecho Comparado 105 <http://www.juridicas.unam.mx/publica/rev/boletin/cont/105/art/art2.htm#P21>
British Medical Association (2004). ‘Human Tissue and Organs – Presumed Consent for Organ Donation’. The Voice of Doctors, May 2004. < http://www.bma.org.uk/ap.nsf/Content/Humantissueorganspresumed>
Caballero, F and López-Navidad, A (2001), ‘For a rational approach to the critical points of the cadaveric donation process’, Transplantation Proceedings 33.
Calabresi, G (1991) ‘Do we own our bodies?’, Health Matrix 1.
Campion-Vincent, V (2000), ‘Les Recits et La Legende des Vols D’Organes, Expression des Reticences Face a la Greffe’, in Carvais, R and Sasportes M (eds) La Freffe humaine. Incertitudes Éthiques: Du Don de Soi à la Ttolérance de L’Autre (Paris : PUF).
Carvais, R and Sasportes, M (eds) (2000) La Greffe Humaine. Incertitudes Éthiques: Du Don de Soi à la Tolérance de L’Autre (Paris : PUF).
Claeys, A and Huriet, C (1999) ‘L’Application de la Loi n°94-654 du 29 Juillet 1994 Relative au Don et a L’Utilisation des Elements et Products du Corps Humain, a L’Assistance Medicale a la Procreation et au Diagnostic Prenatal’ (Office Parlementaire d’Evaluation des Choix Scientifiques et Technologiques).
Consentimiento presunto - Modificaciones a la Ley Nº24.193. Proyecto de Ley, Buenos Aires, 25 de febrero de 2003 <http://www.incucai.gov.ar>
Council of Europe (2002) ‘Additional Protocol to the Convention on Human Rights and Biomedicine, on Transplantation of Organs and Tissues of Human Origin’ <http://conventions.coe.int/Treaty/EN/Treaties/Html/186.htm>
Durkheim, E (1968), Des Formes Élémentaires de la Vie Religieuse (Paris: PUF).
Gnant, M F X and Muhlbacher, F (1990), ‘Kidney Transplantation: Getting the Numbers Right’, The Lancet 335.
Kennedy, I, Sells, R A, Daar, A S, Guttman, R D, Hoffenberg R, Lock, M, Radcliffe-Richards, J and Tilney, N (1998), ‘The case for ‘presumed consent’ in organ donation’, The Lancet 351.
Kittur, D S, Hogan, M M, Thukral V K, McGaw, L J and Alexander, J W, for the United Network for Organ Sharing Ad Hoc Donations Committee (1991), ‘Incentives for organ donation?’, The Lancet 338.
Kluge, E H (2000), ‘Improving Organ Retrieval Rates: Various Proposals and Their Ethical Validity’, Health Care Analysis 8.
Macauley, S (1963), ‘Non-Contractual Relations in Business’, American Sociological Review 28.
Machado, N (1998) Using the Bodies of the Dead Legal, Ethical and Organisational Dimensions of Organ transplantation (Ashgate).
Matesanz, R (2001) ‘A Decade of Continuous Improvement in Cadaveric Organ Donation: The Spanish Model’, Nefrologia XXI.
Matesanz Acedos, R and Fernandez Lucas, M (1996) ‘Actividad de Donacion y Trasplante Pediatrico en España’, Anales Españoles de Pediatria 45.
Michelsen, P (1996) ‘Presumed Consent to Organ Donation: Ten Years Experience in Belgium’, Journal of the Royal Society of Medicine 89.
Parsons, T, Fox, R and Lidz, V (1972), ‘The ‘Gift of Life’ and its Reciprocation’, Social Research 39.
Roels, L et al (1990) ‘Effect of A Presumed Consent Law on Organ Retrieval in Belgium’, Transplantation Proceedings 22.
Roels, L et al (1991) ‘Three Years of Experience with A ‘Presumed Consent’ Legislation in Belgium’, Transplantation Proceedings 23 .
Schneider, W (1999) ‘’Death is Not the Same Always and Everywhere’ Socio-cultural Aspects of Brain Death and the Legislation of Organ Transplantation: The Case of Germany’, European Societies 3.
Scheper-Hughes, N (2000) ‘The Global Traffic in Human Organs’, Current Anthropology 2.
Somerville, M A (1985) ‘’Procurement’ vs ‘Donation’ – Access to Tissues and Organs for
Transplantation: Should ‘Contracting-out’ Legislation be Adopted?’, Transplantation Proceedings 17.
Thouvenin, D (1997) ‘Don et/ou Prelevement D’Organes’, Sciences Sociales et Sante 1.
Voragine, J (1969) The Golden Legend (New York: Arno Press).
Waissmann, R (1996) ‘Analyse des Acceptations et des Refus du Don D’Organes, Une Etude de Cas en France’, Sociologie et Sociétés 2.
Weber, M (1971) Economie et Société (Paris : Plon).
World Health Organisation (1991) Human Organ Transplantation. A Report on Developments Under the Auspices of the WHO (1987-1991) (Geneva: WHO).
