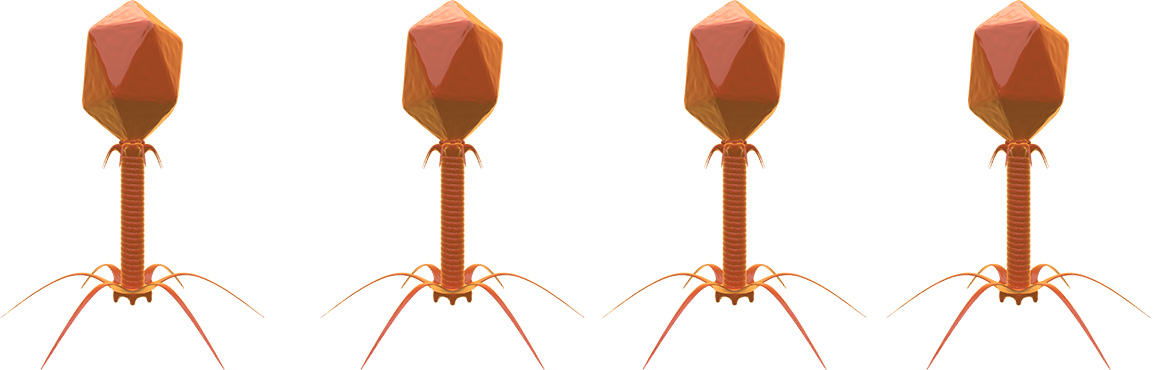
Going viral: What are bacteriophages and how can they help us?
Antibiotics are going to stop working. Bacteria are developing resistance to the drugs we have to treat them and there is no doubt that without action, catching tonsillitis, getting an infection or having surgery is going to get a lot more risky. With a global health crisis on our hands, scientists across the world are now trying to find alternatives to the drugs which have kept us alive for the past decade.
One possible solution is the use of bacteriophages. They sound a bit alien, they even look a bit alien, but these microscopic soldiers could hold the key to fighting some of the most deadly bacteria when our current antimicrobial drugs eventually fail.
Dr Antonia Sagona is a researcher in the School of Life Sciences at Warwick, working on understanding how phages fight infections.
Bacteria devourers
She explains: “Bacteriophages or phages, are viruses that can specifically infect bacteria. The name literally means ‘bacteria devourer’ and they work by parasitizing bacterial cells eating them from the inside out. Bacteriophages are abundant on earth and are present in the areas where their hosts are present. One of the most important structural elements of a bacteriophage is the tail fibres, which make each phage type specific to its host bacteria.
“Due to their ability to tackle bacteria, bacteriophages can be used as antibacterials. Phages have a small genome, so, with recent advances in synthetic biology we can modify them, selecting preferred characteristics and tailoring them for different applications.
“They are now being used for a range of different jobs in bio-detection, industrial applications and food technology and we are currently working on those directions as well. But the most important current focus is developing phages for use in the medical world.”
Using an old idea to solve a modern problem
The use of bacteriophages for therapeutic applications against their host bacteria is called ‘phage therapy’. It sounds very modern but it is not a new idea.
Dr Sagona continues: “Phages were officially discovered by Frederick Twort and Felix d’Herelle in 1915-1917 and they have been used ever since as therapeutics, especially in countries like Russia and Georgia. The reason why phage therapy was abandoned in Western civilization, was mostly because of the discovery of antibiotics – in 1928 penicillin was discovered and from the 1940s onwards more and more antibiotics emerged. These drugs have been highly efficient in clearing bacterial infections and saving lives.
“But since the 1990s, the problem of antibiotic resistance has emerged and the idea of phage therapy has come back into focus.”
Success stories already
Phage therapy can be applied, in principle, to treat any bacterial infection for which a specific phage is present. Examples of infections that are already treated with phage therapy include urinary tract infections, meningitis, gastrointestinal infections, staphylococcal skin diseases and more.
Dr Sagona explains: “There have been real success stories where phage therapy has been used, like the treatment of a 15-year-old patient with cystic fibrosis who had a disseminated Mycobacterium abscessus infection. The patient received an intravenous cocktail of genetically modified bacteriophages with excellent results . This shows the great potential that phage therapy has, especially as bacteriophages can be modified to be safer and more efficient for the treatment of patients.
“In UK, more and more people are interested in phage therapy now and there is discussion about the establishment of hospitals for the use of phages therapeutically, as is the case in other countries including Finland, Brussels, Georgia, Russia and the USA.
“There are a great many advantages to phage therapy, including the fact that it is very specific and efficient. There are very few side-effects and generally phages are easily available, as they are found in nature and we can genetically modify them to make them even better. Additionally, because phages can be mutated along bacteria we have the potential to respond well to possible phage-resistant bacteria”
What’s stopping us using phage therapy?
So if it has proven to be so successful, why don’t we use phage therapy more extensively?
Dr Sagona explains: “There are still some issues to iron out when it comes to phage therapy. Since phages are viruses, there are some ethical limitations on their use therapeutically. There is the potential for some patients to suffer an immune response and there are still difficulties in determining the clinical dose. Also phages rapidly release toxins when they are active we need to understand more about the cellular mechanisms that govern phage therapy.
“All these limitations though can be addressed and research is tackling this every day. We are now showing how bacteriophage enter and interact with human cells and intracellular pathogenic bacteria. More research is available on the potential of immune response upon phage application. When it comes to clinical dose determination, we have shown that work towards encapsulation of bacteriophages in liposomes that are pH-dependent and that enable the release of the phage specifically on the targeted organ, can provide the solution. It is obvious bacteriophages have huge potential to provide the solution to the problem of antimicrobial resistance. Advances in medical technology continue to enable scientists to accelerate research in this field and help make phage therapy a real alternative to antibiotics which we will be able to use even more successfully in the future.
 Dr Sagona is among the scientists speaking at a the next Science on the Hill event at Warwick's Gibbet Hill campus.
Dr Sagona is among the scientists speaking at a the next Science on the Hill event at Warwick's Gibbet Hill campus.
The Rise of the Superbugs: Will your next infection kill you?
10 December 2019 from 18:00 - 20:00
For more information: scienceonthehill@warwick.ac.uk
Published:
3 December 2019
About:
 Dr Antonia Sagona is a research biologist working to investigate the cell biological mechanisms behind bacterial infection and phage therapy and to optimize phages to be safe for phage therapy.
Dr Antonia Sagona is a research biologist working to investigate the cell biological mechanisms behind bacterial infection and phage therapy and to optimize phages to be safe for phage therapy.
Terms for republishing
The text in this article is licensed under a Creative Commons Attribution 4.0 International License (CC BY 4.0).
Share