Variants
 As the COVID-19 pandemic continues there is an ever-present risk of more variants of concern (VOCs) arising. These VOCs may have beneficial mutations aiding their spread. Quickly assessing a substantial change in the risk of infection, morbidity and mortality posed by a new SARS-CoV-2 variant is challenging, with no simple relationship to describe the interactions between any novel variant, disease control policy, adherence to interventions and the historic patterns of infection and vaccination.
As the COVID-19 pandemic continues there is an ever-present risk of more variants of concern (VOCs) arising. These VOCs may have beneficial mutations aiding their spread. Quickly assessing a substantial change in the risk of infection, morbidity and mortality posed by a new SARS-CoV-2 variant is challenging, with no simple relationship to describe the interactions between any novel variant, disease control policy, adherence to interventions and the historic patterns of infection and vaccination.
The COVID pandemic in the UK has been shaped by three main variants of the virus: the wildtype for most of 2020, the alpha variant from October 2020 to May 2021 and the delta variant from March 2021 onwards - with the alpha and delta variant both associated with a substantial increase in transmission. Work from the Zeeman Institute (in strong collaboration with members of the JUNIPER consortium) has been instrumental in determining the rise of these new variants and their likely impact on the pandemic. Research has also focused on the potential impact of future variants especially those that could lead to vaccine escape.
Our publications and pre-prints on variants of COVID are:
| Cavallaro M, Dyson L, Tildesley MJ, Todkill D, Keeling MJ (2023) Spatio-temporal surveillance and early detection of SARS-CoV-2 variants of concern: a retrospective analysis. J. Roy. Soc. Interface 10.1098/rsif.2023.0410 |
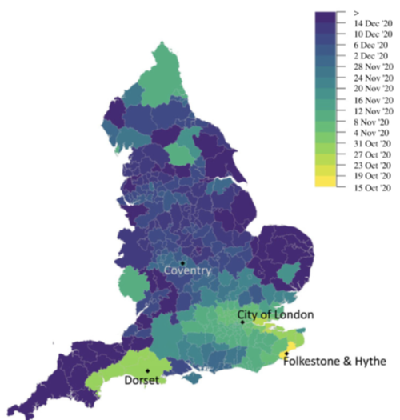 The SARS-CoV-2 pandemic has been characterized by the repeated emergence of genetically distinct virus variants of increased transmissibility and immune evasion compared to pre-existing lineages. In many countries, their containment required the intervention of public health authorities and the imposition of control measures. While the primary role of testing is to identify infection, target treatment, and limit spread (through isolation and contact tracing), a secondary benefit is in terms of surveillance and the early detection of new variants. Here we study the spatial invasion and early spread of the Alpha, Delta and Omicron (BA.1 and BA.2) variants in England from September 2020 to February 2022 using the random neighbourhood covering (RaNCover) method. This is a statistical technique for the detection of aberrations in spatial point processes, which we tailored here to community PCR (polymerase-chain-reaction) test data where the TaqPath kit provides a proxy measure of the switch between variants. Retrospectively, RaNCover detected the earliest signals associated with the four novel variants that led to large infection waves in England. With suitable data our method therefore has the potential to rapidly detect outbreaks of future SARS-CoV-2 variants, thus helping to inform targeted public health interventions.
The SARS-CoV-2 pandemic has been characterized by the repeated emergence of genetically distinct virus variants of increased transmissibility and immune evasion compared to pre-existing lineages. In many countries, their containment required the intervention of public health authorities and the imposition of control measures. While the primary role of testing is to identify infection, target treatment, and limit spread (through isolation and contact tracing), a secondary benefit is in terms of surveillance and the early detection of new variants. Here we study the spatial invasion and early spread of the Alpha, Delta and Omicron (BA.1 and BA.2) variants in England from September 2020 to February 2022 using the random neighbourhood covering (RaNCover) method. This is a statistical technique for the detection of aberrations in spatial point processes, which we tailored here to community PCR (polymerase-chain-reaction) test data where the TaqPath kit provides a proxy measure of the switch between variants. Retrospectively, RaNCover detected the earliest signals associated with the four novel variants that led to large infection waves in England. With suitable data our method therefore has the potential to rapidly detect outbreaks of future SARS-CoV-2 variants, thus helping to inform targeted public health interventions.|
Keeling MJ (2022) Patterns of reported infection and reinfection of SARS-CoV-2 in England. J. Theo. Biol. 10.1016/j.jtbi.2022.111299Link opens in a new window |
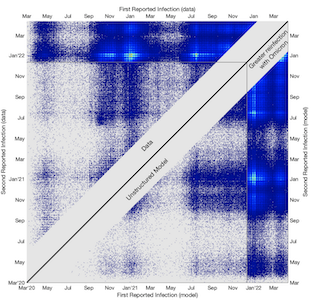 During the early waves of SARS-CoV-2, the underlying paradigm was for long-lasting immunity, but more recent data and in particular the 2022 Omicron waves have shown that reinfection can be relatively common. Here we investigate reported SARS-CoV-2 cases in England, partitioning the data into four main waves, and consider the temporal distribution of first and second reports of infection. We show that a simple low-dimensional statistical model of random (but scaled) reinfection captures much of the observed dynamics, with the value of this scaling providing information of underlying epidemiological patterns. We conclude that there is considerable heterogeneity in risk of reporting reinfection by wave, age-group and location. The high levels of reinfection in the Omicron wave (we estimate that 18% of all Omicron cases had been previously infected, although not necessarily previously reported infection) point to reinfection events dominating future COVID-19 dynamics.
During the early waves of SARS-CoV-2, the underlying paradigm was for long-lasting immunity, but more recent data and in particular the 2022 Omicron waves have shown that reinfection can be relatively common. Here we investigate reported SARS-CoV-2 cases in England, partitioning the data into four main waves, and consider the temporal distribution of first and second reports of infection. We show that a simple low-dimensional statistical model of random (but scaled) reinfection captures much of the observed dynamics, with the value of this scaling providing information of underlying epidemiological patterns. We conclude that there is considerable heterogeneity in risk of reporting reinfection by wave, age-group and location. The high levels of reinfection in the Omicron wave (we estimate that 18% of all Omicron cases had been previously infected, although not necessarily previously reported infection) point to reinfection events dominating future COVID-19 dynamics.|
Hart WS, Miller E, Andrews NJ, Waight P, Maini PK, Funk S, Thompson RN. (2022) Generation time of the alpha and delta SARS-CoV-2 variants: an epidemiological analysis. Lancet Inf. Dis. 10.1016/S1473-3099(22)00001-9 |
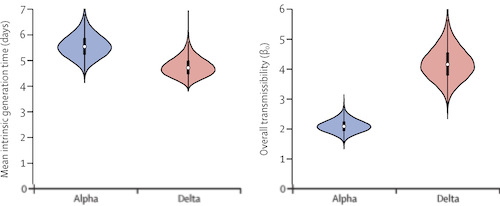 In this paper we analysed transmission data from an ongoing UK Health Security Agency (UKHSA) prospective household study. By fitting a mathematical transmission model to the data, we estimated the intrinsic generation time (which assumes a constant supply of susceptible individuals throughout infection) and the household generation time (which reflects realised transmission in the study households, accounting for susceptible depletion) for the alpha and delta variants. The mean intrinsic generation time was shorter for the delta variant (4·7 days, 95% credible interval [CI] 4·1–5·6) than the alpha variant (5·5 days, 4·7–6·5), with 92% posterior probability. The mean household generation time was 28% (95% CI 0–48%) shorter for the delta variant (3·2 days, 95% CI 2·5–4·2) than the alpha variant (4·5 days, 3·7–5·4), with 97·5% posterior probability.
In this paper we analysed transmission data from an ongoing UK Health Security Agency (UKHSA) prospective household study. By fitting a mathematical transmission model to the data, we estimated the intrinsic generation time (which assumes a constant supply of susceptible individuals throughout infection) and the household generation time (which reflects realised transmission in the study households, accounting for susceptible depletion) for the alpha and delta variants. The mean intrinsic generation time was shorter for the delta variant (4·7 days, 95% credible interval [CI] 4·1–5·6) than the alpha variant (5·5 days, 4·7–6·5), with 92% posterior probability. The mean household generation time was 28% (95% CI 0–48%) shorter for the delta variant (3·2 days, 95% CI 2·5–4·2) than the alpha variant (4·5 days, 3·7–5·4), with 97·5% posterior probability.| Matt J Keeling, Ellen Brooks-Pollock, Robert J Challen, Leon Danon, Louise Dyson, Julia R Gog, Laura Guzman-Rincon, Edward M Hill, Lorenzo M Pellis, Jonathan M Read, Michael J Tildesley. (2021) "Short-term Projections based on Early Omicron Variant Dynamics in EnglandLink opens in a new window" medRxiv. https://doi.org/10.1101/2021.12.30.21268307Link opens in a new window |
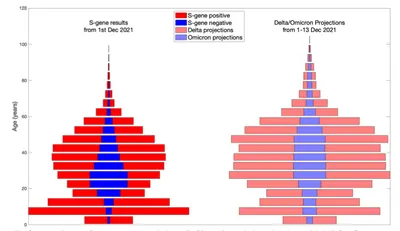 The Omicron variant (B.1.1.529) was first reported to the WHO by South Africa on 24 November 2021 and was declared a variant of concern by the WHO on 26 November 2021. The variant was first detected in the UK on 27 November 2021 and has since been reported in a number of countries globally where it is frequently associated with rapid increase in cases.. We present analyses of UK data showing the earliest signatures of the Omicron variant and mathematical modelling that uses the UK data to simulate the potential impact of this variant in the UK. To account for the uncertainty at the time of writing (December 2021), we include a sensitivity analysis to assess the impact of variant characteristics (transmission advantage, vaccine escape and severity) on future risk.
The Omicron variant (B.1.1.529) was first reported to the WHO by South Africa on 24 November 2021 and was declared a variant of concern by the WHO on 26 November 2021. The variant was first detected in the UK on 27 November 2021 and has since been reported in a number of countries globally where it is frequently associated with rapid increase in cases.. We present analyses of UK data showing the earliest signatures of the Omicron variant and mathematical modelling that uses the UK data to simulate the potential impact of this variant in the UK. To account for the uncertainty at the time of writing (December 2021), we include a sensitivity analysis to assess the impact of variant characteristics (transmission advantage, vaccine escape and severity) on future risk.
 Louise Dyson, Edward M Hill , Sam Moore, Jacob Curran-Sebastian, Michael J Tildesley, Katrina A Lythgoe, Thomas House, Lorenzo Pellis, Matt J Keeling. (2021) "Possible future waves of SARS-CoV-2 infection generated by variants of concern with a range of characteristics" Nature Communications 12: 5370. https://www.nature.com/articles/s41467-021-25915-7 Louise Dyson, Edward M Hill , Sam Moore, Jacob Curran-Sebastian, Michael J Tildesley, Katrina A Lythgoe, Thomas House, Lorenzo Pellis, Matt J Keeling. (2021) "Possible future waves of SARS-CoV-2 infection generated by variants of concern with a range of characteristics" Nature Communications 12: 5370. https://www.nature.com/articles/s41467-021-25915-7 |
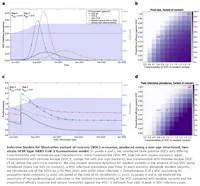 We used three mathematical models to examine the potential drivers of SARS-CoV-2 VOC epidemics in England. We found epidemiological trajectories for putative VOCs are wide-ranging and dependent on their transmissibility, immune escape capability, and the introduction timing of a postulated VOC-targeted vaccine. In particular, a variant that is less transmissible, but shows partial immune-escape, could provoke a wave of infection that would not be revealed until control measures are further relaxed.
We used three mathematical models to examine the potential drivers of SARS-CoV-2 VOC epidemics in England. We found epidemiological trajectories for putative VOCs are wide-ranging and dependent on their transmissibility, immune escape capability, and the introduction timing of a postulated VOC-targeted vaccine. In particular, a variant that is less transmissible, but shows partial immune-escape, could provoke a wave of infection that would not be revealed until control measures are further relaxed.
Figure: (Click for a larger version) Infection burden for illustrative variant of concern (VOC) scenarios, produced using a non-age structured, two-strain SEIR-type SARS-CoV-2 transmission model.
|
Thompson RN, Hill EM, Gog JR. (2021) SARS-CoV-2 incidence and vaccine escape Lancet Inf. Dis., S1473-3099:00202-4. DOI: 10.1016/S1473-3099(21)00202-4 |
A key component of any plausible strategy towards the permanent removal of non-pharmaceutical interventions (NPIs) is ensuring low case numbers in the short to medium term using NPIs and vaccination. Assuming a fixed vaccine escape mutation probability per infection (p), the risk of a vaccine escape variant arising in a specified time period is 1 – (1 – p)N, where N represents the number of cases in that period. Crucially, this expression indicates that the vaccine escape risk is sensitive to background incidence; the risk of an escape variant appearing within a fixed time is an increasing function of incidence (figure). Reducing cases is not only beneficial for decreasing the pressure on health-care systems, but also for lowering the vaccine escape risk.
| Robert Challen, Ellen Brooks-Pollock, Jonathan M Read, Louise Dyson, Krasimira Tsaneva-Atanasova, Leon Danon. (2021) "Risk of mortality in patients infected with SARS-CoV-2 variant of concern 202012/1: matched cohort study" BMJ, 372 (579). https://doi.org/10.1136/bmj.n579 |
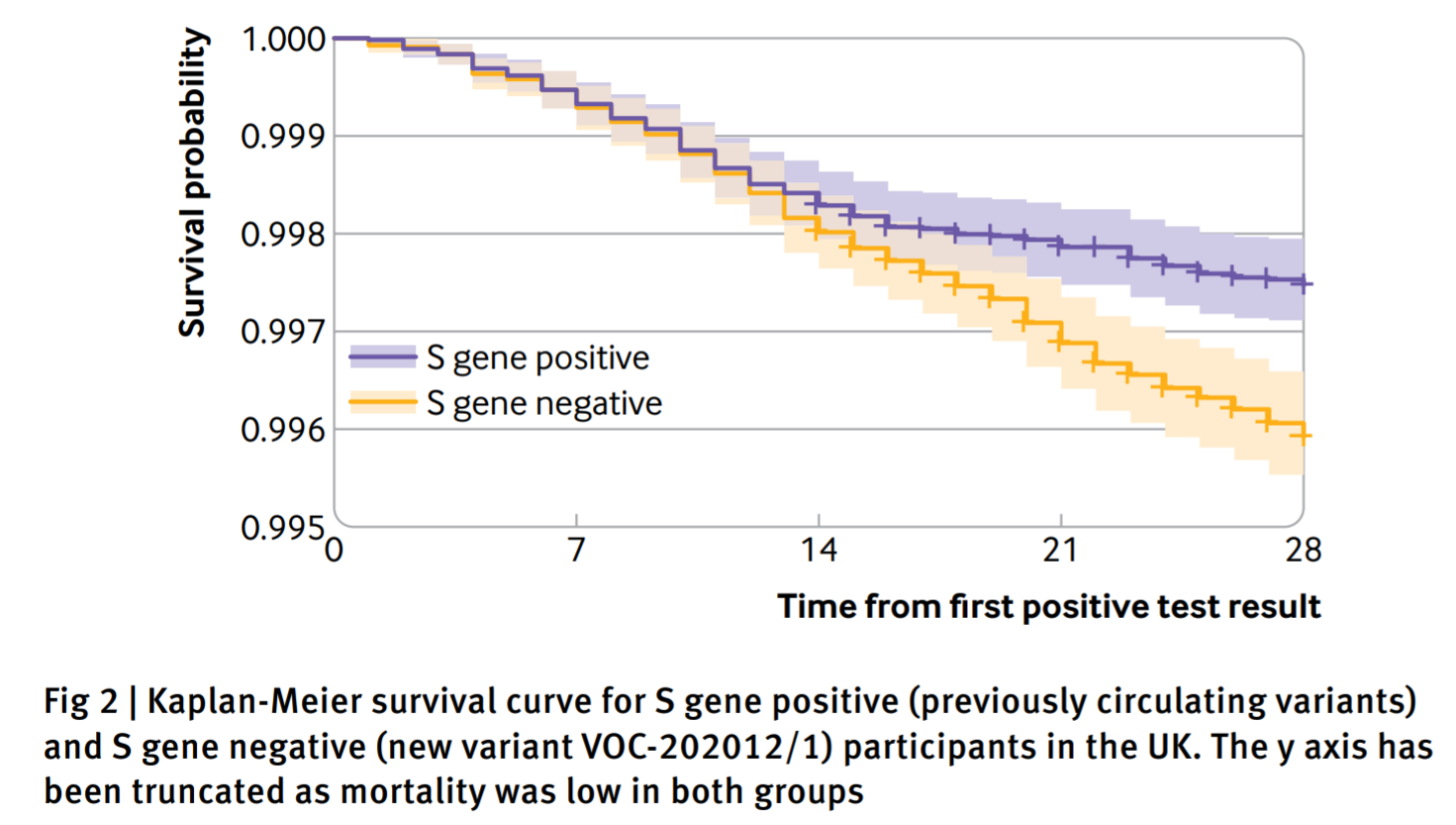 This paper considered the early outbreak data on the Alpha variant, to assess the risk of mortality compared with the originally wildtype variant. Matching by age, sex, ethnicity and location individuals who tested positive for wildtype and Alpha, we were able to account for the change in variant alone. This showed a 64% increase in mortality associated with the Alpha variant, increasing the death rate from 2.5 per 1000 detected cases to 4.1 per 1000.
This paper considered the early outbreak data on the Alpha variant, to assess the risk of mortality compared with the originally wildtype variant. Matching by age, sex, ethnicity and location individuals who tested positive for wildtype and Alpha, we were able to account for the change in variant alone. This showed a 64% increase in mortality associated with the Alpha variant, increasing the death rate from 2.5 per 1000 detected cases to 4.1 per 1000.
| Robert Challen, Louise Dyson, Christopher E. Overton, Laura M. Guzman-Rincon, Edward M. Hill, Helena B. Stage, Ellen Brooks-Pollock, Lorenzo Pellis, Francesca Scarabel, David J. Pascall, Paula Blomquist, Michael Tildesley, Daniel Williamson, Stefan Siegert, Xiaoyu Xiong, Ben Youngman, Juniper, Jonathan M. Read, Julia R. Gog, Matthew J. Keeling, Leon Danon. (2021) " Early epidemiological signatures of novel SARS-CoV-2 variants: establishment of B. 1.617. 2 in England" (medRxiv) https://doi.org/10.1101/2021.06.05.21258365 |
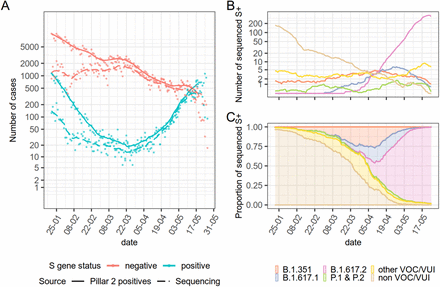 Here we consider the early data on the Delta variant looking at its transmission advantage compared to the Alpha variant - leading from a transition from a declining epidemic to an increasing one. We use a variety of different methods to calculate real-time growth estimates of S-gene positive (likely Delta) cases compared to S-gene negative (likely Alpha) cases and show a sustained, consistent advantage of Delta over Alpha in multiple regions of England. We use the normalisation of age distributions to argue that this transmission advantage is inherent to the Delta variant and is not a result of early higher transmission in specific subpopulations.
Here we consider the early data on the Delta variant looking at its transmission advantage compared to the Alpha variant - leading from a transition from a declining epidemic to an increasing one. We use a variety of different methods to calculate real-time growth estimates of S-gene positive (likely Delta) cases compared to S-gene negative (likely Alpha) cases and show a sustained, consistent advantage of Delta over Alpha in multiple regions of England. We use the normalisation of age distributions to argue that this transmission advantage is inherent to the Delta variant and is not a result of early higher transmission in specific subpopulations.
 See our introductory article on "The Delta variant: What do we know?" courtesy of our friends at +plus magazine.
See our introductory article on "The Delta variant: What do we know?" courtesy of our friends at +plus magazine.