WITHIN Blog: March 2021
A Breath of Fresh Air: Sleep Apnoea & Chronic Pain
By Bruno Saconi, Visiting Research Student in Psychology & the Warwick Sleep & Pain Lab
12/03/2021
Obstructive Sleep Apnoea is a sleep condition that is characterized by repeated episodes of short stops/starts in breathing while asleep. When these occur, oxygen levels drop which is sensed by the brain causing people to wake up frequently throughout the night. The condition is estimated to effect around 8 million people aged 30-69 in the UK, and is highly comorbid with chronic pain conditions. In this month’s blog, guest-written by Bruno Saconi from University of Pennsylvania, we explore the association between obstructive sleep apnoea and chronic pain, as well as some interesting research in this area.
What is Obstructive Sleep Apnoea (OSA)?
There are different types of sleep apnoea, but obstructive sleep apnoea is the most common. In obstructive sleep apnoea (OSA, from now on), breathing pauses are due to intermittent relaxation of the throat muscles that lead to partial or complete obstruction of the airway during sleep.
Box 1. OSA in detail...
Prevalence: In the UK approximately 8 million people aged 30-69 years have OSA. Worldwide prevalence is estimated at one billion. Risk factors include being male, obesity, family history of OSA or snoring, large tonsils and/or neck circumference, and post-menopausal status in females.
Symptoms: Loud snoring, excessive daytime sleepiness, breathing pauses, morning headaches, mood changes, and impotence.
Diagnostic Criteria: Based on an overnight sleep study that may be conducted at a sleep lab (polysomnography) or in the comfort of your home (home sleep apnoea test).
When OSA is undiagnosed or left untreated it is associated with serious health problems including strokes, heart disease, high blood pressure, and diabetes (Solomon et al., 2019). People with OSA are often sleepy, which places them at higher risk for road collisions and work-related injuries (Gurubhagavatula et al., 2017). Despite this, it is estimated that up to 90% of adults remain undiagnosed, and therefore untreated (Punjabi, 2008).
At this point, you might be worried about OSA, especially if you or a loved one has these symptoms or been diagnosed with OSA. Some positive news is that there are multiple effective treatment options available. The recommended approach for treating moderate to severe OSA is continuous positive airway pressure (CPAP or just PAP). A CPAP machine delivers continual air pressure to your airway through a mask worn over your nose/mouth region while you sleep. The air provided by the CPAP ‘supports’ the airway to keep it free from collapse. This prevents the temporary stop in breathing whilst sleeping which in turn stops the individual from waking up – meaning people are able to have longer and better-quality sleep.
Fig 1. Example of a CPAP Machine for OSA
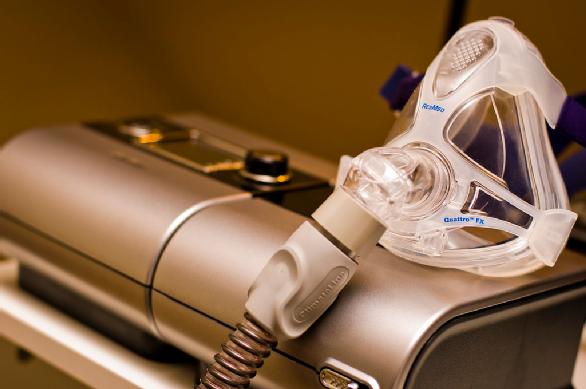
Photo Credit: Pete Prodoehl VIA PhotoPin
Sleep Apnoea & Pain:
As previously highlighted in our blog "Can Catching Z's Relieve Pain?" we know that sleep and pain are related, and that sleep problems and chronic pain frequently co-occur. This is also true with OSA. People with OSA are more reactive to pain and tend to report higher pain intensity than those without OSA (Charokopos at al., 2018).
-
Approximately 32% of adults with chronic pain also have OSA (Mathias et al., 2018).
-
Among patients with OSA, prevalence of chronic pain ranges from 55.4% (Aytekin et al., 2015) to 76.2% (Mundt et al., 2017).
As there is evidence to suggest that OSA and chronic pain co-occur, you might be wondering why they aren’t treated simultaneously. Findings from a growing number of studies have suggested that there are some possible benefits of applying continual positive air pressure to pain & comorbid OSA (Charokopos at al., 2018). Khalid et al. (2011) evaluated the effects of CPAP on sensitivity to pain in twelve patients with severe OSA. Participant were instructed to use the prescribed CPAP treatment nightly for 6-8 weeks at home. Within this time, they returned to the sleep center for further pain sensitivity assessments. The results showed CPAP improved sleep continuity and reduced pain sensitivity in patients with severe OSA.
These findings were supported by another study that found that CPAP treatment improved both sleep quality and pain tolerance in elderly patients with OSA (Onen et al., 2010). This suggests that treating OSA – a sleep disorder – may be an opportunity to better manage chronic pain. However, it is worth noting that these initial findings are largely based on small-scale study that only recruited people with OSA and no pre-existing chronic pain. Therefore, further research is required in a chronic pain population.
 Photo Credit: PEXELS VIA PIXABAY
Photo Credit: PEXELS VIA PIXABAY
While we don’t fully understand the OSA-chronic pain association just yet, here at the Warwick Sleep & Pain Lab, members of our research team are investigating this relationship. Specifically, we are interested in how cognitive-behavioral factors (e.g., sleep-related anxiety, beliefs about the sleep-pain interaction) and coping strategies could influence pain and sleep in people with OSA and comorbid chronic pain. If you or someone you know has been diagnosed by a healthcare professional with OSA & chronic pain, or you believe you experience these conditions, you might be eligible for one of our planned studies due to launch in 2021 - Eligible adults will complete an online questionnaire and participants will be compensated for their time. For more information, keep an eye on the upcoming Sleep & Pain Lab newsletters or email Bruno Saconi via the details at the end of this blog!
Finally, if you are concerned about your sleep, or worry you could have OSA, please talk to your GP or primary healthcare provider, and check out some of the links at the end of this blog which may also be of use to you. Healthy sleep is an essential pillar for a healthy life!

Written by Bruno Saconi, PhD Candidate at the University of Pennsylvania, School of Nursing (USA)
& Visiting Research Student in Psychology at the University of Warwick, Sleep and Pain Lab
Do you have OSA and are interested in Bruno's study?
Pre-register your interest...
Email: bsaconi@nursing.upenn.edu
Or sign up to our Warwick Sleep & Pain Lab Volunteers page!
Glossary:
Apnoea – temporary cessation of breathing
Comborbid – In medicine, a comorbidity is the presence of one or more additional conditions which are co-occurring/experienced simultaneously
Pain tolerance – the maximum intensity of a pain-producing stimulus (e.g., thermal, electric) that a person is willing to accept in a given situation. A common measure of pain in experimental research.
Pain sensitivity – the proneness to react to standardized stimuli (e.g., thermal, electric), varies widely from person to person. Another common measure of pain in experimental research.
Useful Links:
British Lung Foundation: https://www.blf.org.uk/support-for-you/osa
NHS: https://www.nhs.uk/conditions/sleep-apnoea/
Sleep Apnoea Trust (UK Charity): https://sleep-apnoea-trust.org/
Pain Concern: https://painconcern.org.uk/
References:
Aytekin, E., Demir, S. E., Komut, E. A., Okur, S. C., Burnaz, O., Caglar, N. S., & Demiryontar, D. Y. (2015). Chronic widespread musculoskeletal pain in patients with obstructive sleep apnea syndrome and the relationship between sleep disorder and pain level, quality of life, and disability. Journal of Physical Therapy Science, 27(9), 2951–2954. https://doi.org/https://dx.doi.org/10.1589/jpts.27.2951
Charokopos, A., Card, M. E., Gunderson, C., Steffens, C., & Bastian, L. A. (2018). The Association of Obstructive Sleep Apnea and Pain Outcomes in Adults: A Systematic Review. Pain Medicine, 19(suppl_1), S69–S75. https://doi.org/10.1093/pm/pny140
Gurubhagavatula, I., Sullivan, S., Meoli, A., Patil, S., Olson, R., Berneking, M., & Watson, N. F. (2017). Management of obstructive sleep apnea in commercial motor vehicle operators: Recommendations of the AASM sleep and transportation safety awareness task force. Journal of Clinical Sleep Medicine, 13(5), 745–758. https://doi.org/10.5664/jcsm.6598
Khalid, I., Roehrs, T. A., Hudgel, D. W., & Roth, T. (2011). Continuous Positive Airway Pressure in Severe Obstructive Sleep Apnea Reduces Pain Sensitivity. Sleep, 34(12), 1687–1691. https://doi.org/10.5665/sleep.1436
Mathias, J. L., Cant, M. L., & Burke, A. L. J. (2018). Sleep disturbances and sleep disorders in adults living with chronic pain: A meta-analysis. Sleep Medicine, 1–13. https://doi.org/10.1016/j.sleep.2018.05.023
Mundt, J., Eisenschenk, S., & Robinson, M. (2017). (396) Severity and likelihood of chronic pain in individuals with obstructive sleep apnea and insomnia. The Journal of Pain, 18(4), S73. https://doi.org/10.1016/j.jpain.2017.02.246
Onen, S. H., Onen, F., Albrand, G., Decullier, E., Chapuis, F., & Dubray, C. (2010). Pain tolerance and obstructive sleep apnea in the elderly. Journal of the American Medical Directors Association, 11(9), 612–616. https://doi.org/10.1016/j.jamda.2010.04.003
Punjabi, N. M. (2008). The epidemiology of adult obstructive sleep apnea. Proceedings of the American Thoracic Society, 5(2), 136–143. https://doi.org/10.1513/pats.200709-155MG
Solomon, C. G., Veasey, S. C., & Rosen, I. M. (2019). Obstructive sleep apnea in adults. New England Journal of Medicine, 380(15), 1442–1449. https://doi.org/10.1056/NEJMcp1816152
Photo Credit:
Fig 1. Pete Prodoehl <a href="http://www.flickr.com/photos/35237092540@N01/6746706041">CPAP</a> via <a href="http://photopin.com">photopin</a> <a href="https://creativecommons.org/licenses/by-nc-sa/2.0/">(license)</a>
