Sarah Drury
human embryo aged 6 days
What got you interested in this area of science?
During my time as an undergraduate at the University of Wolverhampton studying for a BSc (Hons) in Biomedical Sciences, I completed a one-year sandwich placement in the Andrology laboratory at the Assisted Conception Unit (ACU), Birmingham Womens Hospital. During this year, I undertook a research project entitled "Characterisation of apoptotic markers in cumulus cells from individual human oocytes", and presented my findings at a national fertility conference, for which I received the award of "British Fertility Society Best Young Scientist". The experience I gained during my placement made me realise that I wanted to work in the field of reproductive medicine, so once I had graduated I returned to the ACU to resume my career as an Andrologist. I have since trained as an Embryologist, and relocated to the Centre for Reproductive Medicine (CRM) at University Hospitals Coventry and Warwickshire. When the chance of a PhD Fellowship arose, I was keen to take the opportunity to embark on research in reproductive medicine in order to progress academically and ultimately improve the service we provide as Clinical Embryologists. I am currently on a three-year secondment whilst I complete my PhD entitled "Molecular Diagnosis of Human Embryo Viability" at Warwick Medical School.
How is the work you are currently doing relevant to everyday life?
Approximately one in six couples suffers from infertility, with around one third of those currently attending the CRM being diagnosed with "unexplained" infertility. Medical advancements in the field of reproductive medicine have been phenomenal since the birth of the first test tube baby just over 30 years ago, and in vitro fertilisation (IVF) has since become routine medical practice, but with success rates following IVF treatment at around 35% per cycle, there is clearly scope for improvement. One of the major problems associated with IVF treatment is the high incidence of multiple pregnancies, which increases the risk of obstetric and neonatal complications, as well as imposing a higher financial burden on both the NHS and individual families. With the number of babies born following IVF treatment steadily increasing, these are important considerations that must be addressed.
What does your research hope to achieve?
Investigation of the molecular processes that occur within the growing embryo should provide us with a better understanding of embryo development, and enable us to select the single most viable embryo to transfer into the uterus during clinical IVF treatment. At present, selection is based upon the appearance of the embryo at the light microscope level. However, since embryos are assessed at ~24-hourly intervals, many changes occur in between which we do not see. By studying the structural and dynamic changes within the embryo from fertilisation (day 1) through to the blastocyst stage (day 5 or 6) using fluorescent microscopy techniques, we should be able to predict more accurately which embryo will most likely result in a live birth, thus improving the success rate of IVF treatment whilst reducing the incidence of multiple gestations.
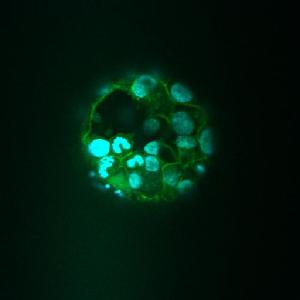
Briefly, what does the image show?
The image shows a human embryo at the blastocyst stage of development, 6 days after fertilisation in vitro, and stained with a fluorescent dye to enable us to see the protein cytoskeleton that helps to maintain the shape of the embryo (green) and the nucleus, containing DNA, of each individual cell within the embryo (blue). The image was obtained by taking an optical section through the embryo using a specialised confocal microscope which uses laser technology to virtually "slice" the embryo very thinly. This allows us to look at structures both inside and on the surface of the embryo in great detail.
for more information please visit: http://www2.warwick.ac.uk/fac/med/research/csri/rh/genesis/