Dr Pasquale F Innominato
Technical summary
I have previously demonstrated that altered circadian rest-activity rhythms, evaluated with wrist-actigraphy monitoring, as well as subjective sleep complaint, whether occurring before or during chemotherapy, are associated with shorter overall survival and poorer quality of life in patients with advanced colorectal cancer.
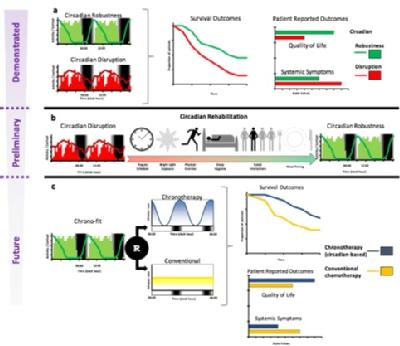 Similar findings have been subsequently reported for the cortisol diurnal rhythm in other cancer types. Taken together, these data underpin the clinical relevance of circadian rhythm assessment in cancer patients, and constitute the basis for an integrative and innovative therapeutic approach, aimed at restoring robust circadian function in cancer patients. Based on experimental models and data in other diseases, I expect that the reconstitution of normal circadian function would improve both the outcome and the well-being of cancer patients. In order to achieve this objective, I foresee integrating pharmacological and behavioural personalised interventions. Hence, the optimisation of such approach requires the incorporation, within a systems medicine framework, of basic science, translational studies, observational and interventional clinical trials, alongside biomedical technology development for seamless, continuous and insightful home monitoring of cancer patients receiving chemotherapy.
Similar findings have been subsequently reported for the cortisol diurnal rhythm in other cancer types. Taken together, these data underpin the clinical relevance of circadian rhythm assessment in cancer patients, and constitute the basis for an integrative and innovative therapeutic approach, aimed at restoring robust circadian function in cancer patients. Based on experimental models and data in other diseases, I expect that the reconstitution of normal circadian function would improve both the outcome and the well-being of cancer patients. In order to achieve this objective, I foresee integrating pharmacological and behavioural personalised interventions. Hence, the optimisation of such approach requires the incorporation, within a systems medicine framework, of basic science, translational studies, observational and interventional clinical trials, alongside biomedical technology development for seamless, continuous and insightful home monitoring of cancer patients receiving chemotherapy.
Furthermore, my research interest is to optimise the schedule of administration of anticancer drugs according to the circadian rhythms of each individual patient. A standard, unified approach has demonstrated a clinical benefit only in a subgroup of patients, possibly because of chemotherapy-induced circadian disruption has not been fully accounted for. Therefore, through the integration of effective and adaptive dynamic monitoring of circadian function, and personalised delivery models determined within a systems biology approach, I envision that chronotherapeutics will eventually benefit most of the patients on anticancer treatment.
The combination of circadian function restoration and circadian-based administration of anticancer drugs would ultimately lead to a wider therapeutic index of chemotherapy, thus to less toxicity, higher efficacy, better quality of life and less severe symptoms.
Selected publications:
- Innominato PF, Lim AS, Palesh O, Clemons M, Trudeau M, Eisen A, Wang C, Kiss A, Pritchard KI, Bjarnason GA. The effect of melatonin on sleep and quality of life in patients with advanced breast cancer. Support Care Cancer. 2016 Mar;24(3):1097-105. doi: 10.1007/s00520-015-2883-6. PMID: 26260726.
- Innominato PF, Spiegel D, Ulusakarya A, Giacchetti S, Bjarnason GA, Lévi F, Palesh O. Subjective sleep and overall survival in chemotherapy-naïve patients with metastatic colorectal cancer. Sleep Med. 2015 Mar;16(3):391-8. doi: 10.1016/j.sleep.2014.10.022. PMID: 25678361.
- Ortiz-Tudela E, Iurisci I, Beau J, Karaboue A, Moreau T, Rol MA, Madrid JA, Lévi F, Innominato PF. The circadian rest-activity rhythm, a potential safety pharmacology endpoint of cancer chemotherapy. Int J Cancer. 2014 Jun 1;134(11):2717-25. doi: 10.1002/ijc.28587. PMID: 24510611.
- Innominato PF, Giacchetti S, Moreau T, Smaaland R, Focan C, Bjarnason GA, Garufi C, Iacobelli S, Tampellini M, Tumolo S, Carvalho C, Karaboué A, Lévi F; ARTBC International Chronotherapy Group. Prediction of survival by neutropenia according to delivery schedule of oxaliplatin-5-Fluorouracil-leucovorin for metastatic colorectal cancer in a randomized international trial (EORTC 05963). Chronobiol Int. 2011 Aug;28(7):586-600. doi: 10.3109/07420528.2011.597532. PMID: 21859417.

