Mind Matters

‘Mind Matters’ was a student-led exhibition at the Modern Records Centre, University of Warwick. The exhibition was created by four second year history students – Karima Aqli, Glory Chan, Zaeem Hoque and Khilna Shah. The exhibition was due to be open from 21 April 2020 to 21 May 2020, with an exciting launch event involving talks delivered by professionals and interactive activities. Unfortunately due to the coronavirus pandemic the exhibition did not take place.
The exhibition explored the evolution of mental health care in the UK over the past century from a historical perspective through the unique collections held by the MRC. A wide variety of sources, ranging from official reports and correspondences to popular pamphlets and advertisements were included.
Although the physical exhibition can no longer be installed, the contextual information written by the students is reproduced here.
About Mind Matters
While the issue of mental health is occupying an increasingly significant place at the forefront of our present social consciousness, it is by no means a concern exclusive to our contemporary society. Adopting a historical perspective, this exhibition traces and demonstrates changing attitudes and approaches towards mental health in the UK from the beginning of the 20th century onwards. Starting from the establishment of the Lunacy Act in 1890, it looks at the perceptions of mental illness from both an official and social viewpoint. Officially, there was a gradual shift in approaches to the treatment of mental illnesses, as the institutionalisation of patients with mental illnesses in asylums and psychiatric hospitals slowly transitioned towards the provision of care in the community. Socially, the changing language associated with mental health also evidences the gradual, albeit incomplete, movement towards de-stigmatisation. Additionally, by examining changes in the support for mental health in the University of Warwick itself, this exhibition illustrates how the University, as a microcosm of the wider British society, responded to the aforementioned changes.
Out of Sight, Out of Mind
Asylums and the institutionalisation of patients with mental illnesses
The treatment of mental health disorders has changed throughout the course of the 20th century. The items in this section provide an insight into asylums in 20th century Britain and how people thought mental health disorders should be treated. People who suffered from mental illnesses were admitted into asylums, where they would be provided with an environment in which they could be treated and recover. Asylums not only provided safety for the patient, but also the rest of society. This is because patients were often seen to be as much of a danger to society as they were to themselves. Therefore, there was an element of separation as well as treatment when it came to asylums. The treatment provided in asylums was certainly different to what we have access to today. We now have access to online services, counselling and support groups but this was not the case in the 20th century, when mental illnesses were not treated with the same compassion and empathy. Instead they were often seen as mere diseases that needed to be cured. While the items in the cabinet depict a relatively derelict image of the experience in asylums, it is important to note that a lot of money was invested in them at the time. There was also an effort to train staff in order to appropriately care for patients. Therefore, despite the sparking contrast to the treatment available today, asylums in 20th century Britain were genuinely seen as helpful places for the mentally ill to recover.
Care in the Community
A shift towards de-institutionalisation
With increased criticisms against the effectiveness and morality of institutional care during the mid 1900s, treatment of mental disorders was gradually shifted to the idea of community care, also referred to as de-institutionalisation. Contrary to segregation, which involves placing patients with mental illnesses in psychiatric institutions, community care focuses on integrating mental health patients into the community in domiciliary settings. This meant incorporating mental health services into the NHS, placing responsibility for mental health in the hands of local authorities, and promoting a variety of treatment options such as halfway houses, community mental health centres, self-help groups and outpatient services. Politically, it was hoped that community care would reduce pressures on psychiatric institutions and alleviate problems of rehabilitating patients back into society. Economically, community care was seen as a way to limit public expenditures on psychiatric institutions and provide a more cost-effective option of prevention rather than treatment. Morally, community care was believed to be more humane as patients were given more choices and lessened chances of social exclusion. Clinically, by tailoring treatment to individual needs and making them more accessible, community care was considered to be more effective in addressing mental health problems.
Mind your language
‘Lunatic’, ‘Idiot’, ‘Imbecile’. All terms that are highly unacceptable now but that once had a more medico-legal beginning. Despite the terms now being equal in their nature as an abusive term, up until the mid-twentieth century, they were commonly employed both in the medical and legal fields to refer to people with mental health illnesses. These terms were not equal in value; an ‘idiot’ was not an ‘imbecile’ and by law the rights of a ‘lunatic’ differed from those of an ‘idiot’. Although a distinction between lunacy and idiocy was present from the thirteenth century onwards, this was legally recognised in the 1886 Idiots Act. The term ‘lunatic’, its use traced back to the fourth century, was initially believed to be someone whose mental state was influenced by the phases of the moon. The distinction later came that described lunacy as a temporary acquired mental illness that differed from the permanent mental illness from birth as prevalent in the condition of an ‘idiot’. As present from the Mental Deficiency Act of 1913, terms such as idiocy, imbecility and even moral defectivity were all listed as legitimate legal and medical terminology that aimed to categorise and classify those who experienced mental illnesses. Imbecility was also not limited to those who experienced mental health issues but rather anyone who displayed any form of social deviance or immorality. But by the 1960s, it was clear to see that the once medico-legal term had entered the public domain and become an insult in of itself. To be a ‘lunatic’, an ‘idiot’ or an ‘imbecile’, i.e. someone who had a mental health condition, was seen as ‘undesirable’ and thus as an insult.
Linked to the ideas of degeneration, desirability and social Darwinism, people who suffered from ‘mental deficiency’ became the target of the eugenics movement. From segregation to sterilisation, the societal stigmatisation of mental health is ever prevalent in the evolution of the terms from its medico-legal beginning to its acquired derogative meaning. By the 1960s is it really as the WHO claims? Has the fear of the ‘madman’ really been conquered?
University of Warwick
A response to changing perceptions of mental health
Mental health has been a pertinent issue facing campuses all over the world for many years. In contemporary Britain there has been a significant spike in mental health disorders including anxiety and depression. In the 12 months ending July 2017, the rate of suicide for university students in England and Wales was 4.7 deaths per 100,000 students, which equates to 95 suicides or about one death every four days. This statistic illustrates how much of a crisis mental health is on campus. As undergraduates at the University of Warwick it is fascinating to see the measures put in place to mitigate mental health issues and observe the support offered to those suffering. From our research, we have identified there has definitely been a change in attitudes and there is a lot more support now than ever before. Our hypothesis for the reason for this change is because there has been improvements and advances in medical research and this has reduced the stigma at a societal level for those suffering with mental health issues. An interesting observation made whilst conducting archival research is the lack of primary sources associated with mental health at the University of Warwick. This demonstrates that historically there was a lack of support and acknowledgement of the crisis that is mental health and this is indicative of sparse amount of sources.
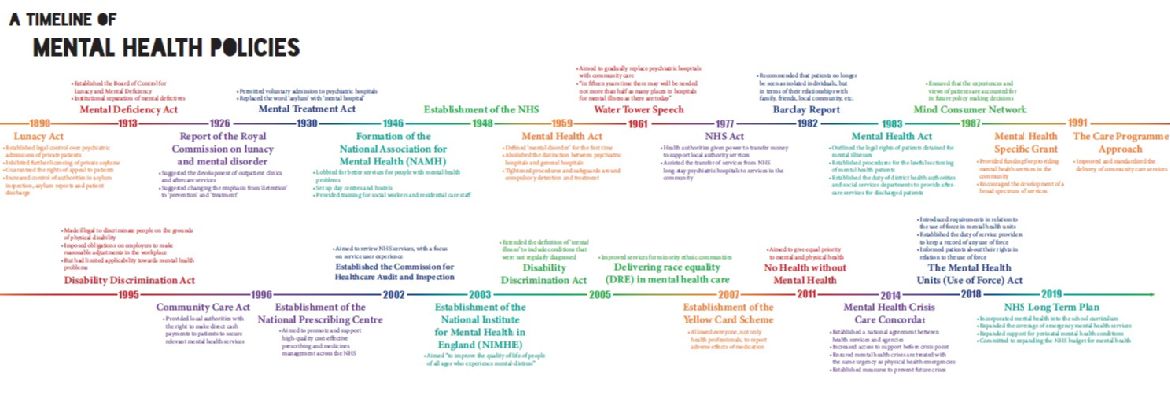
Timeline of mental health policies, 1890-2019
Game:
Can you escape the asylum?
This fun and interactive board game took you through the changing mental health scene from the 20th century to the present-day. The game built upon the exhibition to engage and educate individuals on the changing trends of mental health developments.

Further reading:
Barham, Peter, Closing the Asylum: The Mental Patient in Modern Society, 2nd edn (London: Penguin Books, 1997).
Cherry, Steven ‘Mental health care in modern England: the Norfolk Lunatic Asylum/St. Andrew's Hospital’, 2003
Clarke, Liam, 'The opening of doors in British mental hospitals in the 1950s', History of Psychiatry, 4, (1993), 527-551.
Dickinson, Eileen. “From Madness to Mental Health: A Brief History of Psychiatric Treatments in the UK from 1800 to the Present.” British Journal of Occupational Therapy, vol. 53, no. 10, Oct. 1990, pp. 419–424,
'Historical Attitudes towards Mental Health', People's History of the NHS
Kritsotaki, Despo et al (eds), Deinstitutionalisation and after: post-war psychiatry in the Western world (Switzerland: Palgrave MacMillan, 2016).
'Lunatic Asylums and The Lunacy Laws', The British Medical Journal, vol. 2, no. 87, 1858, pp. 732–733
Scull, Andrew, Decarceration: community treatment and the deviant - a radical view (London: Prentice Hall, 1977).
Taylor, Barbara, 'The Demise of the Asylum in in Late Twentieth-century Britain: A Personal History', Transactions of the Royal Historical Society, 21, (2011), 193-215.
Taylor, Barbara, ‘The Last Asylum: A Memoir of Madness in Our Times’, 2014
'The way universities are run is making us ill: inside the student mental health crisis', The Guardian, 27 September 2019
Thomson, Matthew, 'The Problem of Mental Deficiency; Eugenics, Democracy and Social Policy in Britain c.1870-1959' (United States, New York: Oxford University Press, 1998)
Walker, Carl, Hart, Angie, Hanna, Paul, 'Building a new community psychology of mental health: spaces, places, people and activities' (London: Palgrave MacMillan, 2017).
